Physical Symptoms of Perimenopause by Body System
Physical symptoms of perimenopause affect nearly every body system. Explore how hormonal changes impact your brain, heart, joints, gut, skin, and more — clearly explained, system by system.
EDUCATIONAL
Perimenopause Compass
2/18/202619 min read
Physical Symptoms of Perimenopause by Body System
Your joints ache. Your heart races. Your gut is unpredictable. Your skin is dry. Your brain won't focus. Your sleep is shattered.
You've seen the cardiologist. The rheumatologist. The gastroenterologist. The dermatologist. Maybe even the neurologist. Each one ran tests. Each one said: "Everything looks normal."
But nothing feels normal.
If you're a woman between 40 and 55 and you're collecting symptoms that no single specialist can explain — there's a very good chance they're all connected. And the connection is hormonal.
Perimenopause doesn't just affect your periods. Estrogen and progesterone have receptors in virtually every organ and tissue in your body — your brain, your heart, your bones, your gut, your skin, your immune system. When these hormones fluctuate and decline, the ripple effects are systemic.
This article does something most perimenopause resources don't: it organizes your symptoms by body system — so you can finally see the full picture, understand why each symptom is happening, and stop feeling like your body is mysteriously falling apart.
It's not. It's recalibrating. And once you understand the map, the journey makes a lot more sense.
Why Perimenopause Affects Your Entire Body — Not Just Your Periods
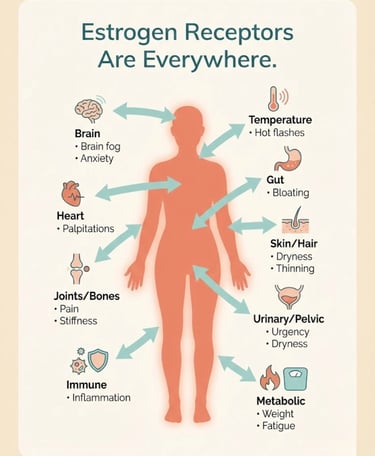
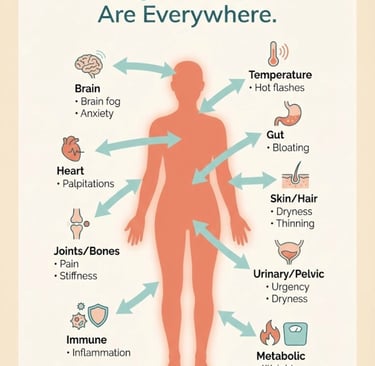
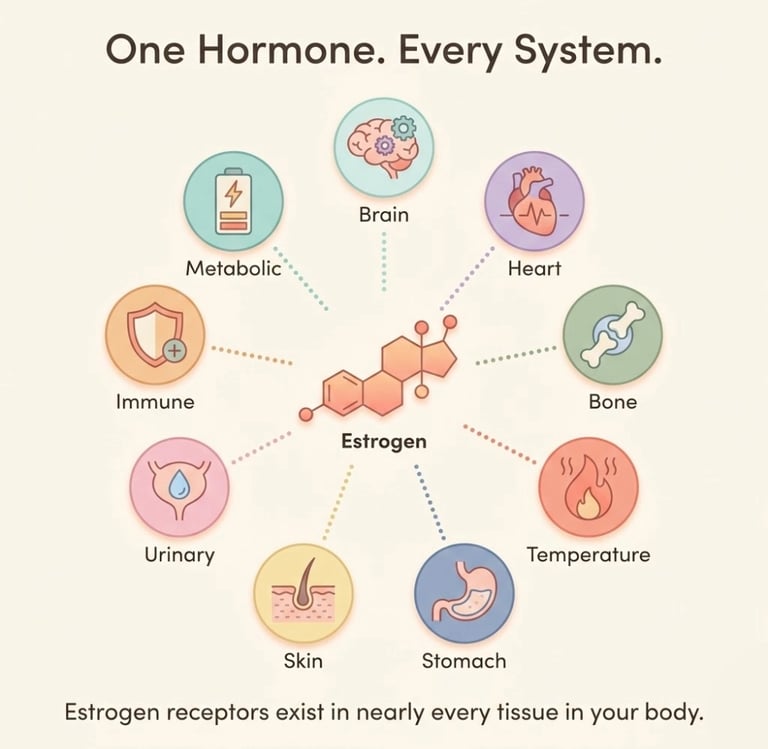
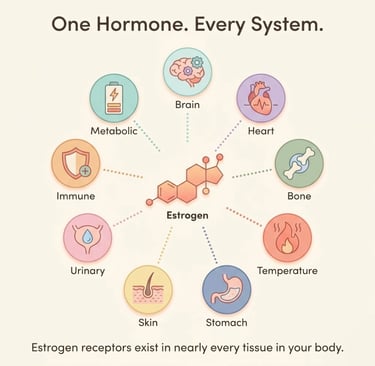
Estrogen Receptors Are Everywhere
Here's the fact that changes everything: estrogen receptors exist in nearly every tissue in the human body.
They're in your:
Brain — affecting mood, cognition, temperature regulation, and sleep
Heart and blood vessels — influencing heart rate, blood pressure, and vascular flexibility
Bones and joints — maintaining bone density and joint lubrication
Gut — regulating motility, microbiome composition, and inflammation
Skin — supporting collagen production, hydration, and elasticity
Urinary tract and vaginal tissue — maintaining tissue health and moisture
Immune system — modulating inflammatory responses
Metabolic organs — affecting insulin sensitivity, fat distribution, and thyroid function
This is why perimenopause produces such a wide range of seemingly unrelated symptoms. They're not unrelated at all. They're all downstream effects of the same hormonal shift — just manifesting in different body systems.
The Domino Effect of Hormonal Instability
During perimenopause, your hormones don't simply decline — they fluctuate wildly and unpredictably. Estrogen can spike to levels higher than your 20s one week, then crash the next. Progesterone drops as ovulation becomes inconsistent.
This instability creates a domino effect across body systems:
Estrogen spike → your brain's thermostat misfires → hot flash
Estrogen crash → serotonin and GABA drop → anxiety and insomnia
Progesterone decline → less GABA enhancement → sleep disruption and restlessness
Cortisol reactivity increases → stress response amplified → palpitations, tension, weight gain
Inflammation rises → joint pain, gut disruption, skin changes → systemic symptoms
No single system operates in isolation. And that's precisely why perimenopause can feel so overwhelming — and why a body-systems approach finally makes it make sense.
Your Brain and Nervous System
Estrogen's role: Estrogen modulates serotonin, dopamine, GABA, acetylcholine, and norepinephrine — the neurotransmitters that regulate mood, memory, attention, calm, and cognitive processing. It also influences the hypothalamus (your body's thermostat and stress response center).
Brain Fog, Memory Lapses, and Word-Finding Difficulty
One of the most distressing — and most common — cognitive symptoms of perimenopause.
What it feels like:
Walking into a room and forgetting why
Losing a word mid-sentence — it's right there but won't come
Reading a paragraph and realizing you absorbed nothing
Difficulty multitasking — something that used to be effortless
Feeling mentally "slow" or like you're thinking through cotton
What's happening: Estrogen supports verbal memory, processing speed, and executive function. The SWAN study confirmed that cognitive changes — particularly in verbal memory and processing speed — are associated with the menopausal transition.
Important reassurance: Perimenopausal brain fog is real, documented, and typically temporary. Research suggests that cognitive function generally recovers after menopause once hormones stabilize at their new baseline. This is not early dementia.
Anxiety, Panic, and the Rewired Stress Response
New-onset anxiety is one of the most underrecognized perimenopause symptoms — because it often appears before any physical changes.
What it feels like:
A sense of dread or impending doom without a trigger
Physical anxiety — tight chest, racing heart, shallow breathing
Ruminating thoughts, especially at night
Feeling "wired but tired"
Panic-like episodes that seem to come from nowhere
What's happening: Estrogen enhances GABA (your brain's calming neurotransmitter) and serotonin (which stabilizes mood). When estrogen fluctuates, these calming systems become less reliable. Your amygdala (the brain's threat-detection center) becomes more reactive. The result: your stress response fires more easily, more intensely, and with less provocation.
Headaches and Migraines — New or Worsening
If you're getting more headaches — or your first-ever migraines — hormones may be the reason.
What's happening: Estrogen fluctuations affect serotonin pathways and blood vessel dilation in the brain. Many women who experienced menstrual migraines find they worsen during perimenopause. Some women who never had migraines develop them for the first time.
Pattern clue: If your headaches cluster around specific points in your cycle (or what remains of it), a hormonal connection is likely.
Dizziness and Sensory Changes
Less discussed but not rare:
Dizziness or lightheadedness — sometimes related to blood pressure changes, sometimes to inner ear sensitivity
Tinnitus (ringing in the ears) — reported by some women during the transition
Changes in taste or smell — subtle but noticeable
Increased sensitivity to light or sound — your nervous system is more reactive
These sensory shifts are thought to be related to estrogen's influence on neural sensitivity and autonomic nervous system regulation.
What Science Says About Estrogen and the Brain
Established:
Estrogen receptors (ERα and ERβ) are abundant in brain regions involved in memory, mood, and thermoregulation
The SWAN study documented measurable cognitive changes during the menopausal transition
Brain fog typically improves after menopause
Probable:
Estrogen may have neuroprotective properties — and the timing of HRT relative to menopause (the "window of opportunity") may matter for long-term cognitive health
The severity of cognitive symptoms during perimenopause may be influenced by cardiovascular health and metabolic factors
Still debated:
Whether perimenopausal hormonal changes have lasting effects on brain aging
The cognitive benefits (or risks) of HRT initiated at different stages
Your Cardiovascular System
Estrogen's role: Estrogen promotes vasodilation (blood vessel flexibility), supports healthy cholesterol profiles, and helps regulate heart rhythm via the autonomic nervous system.
Heart Palpitations — Why Your Heart Races for No Reason
What it feels like:
A sudden fluttering or pounding sensation in your chest
Feeling like your heart "skips a beat"
Racing heartbeat when lying down — especially at night
An awareness of your heartbeat that's uncomfortable
What's happening: Estrogen fluctuations affect the autonomic nervous system — the system that regulates heart rate without your conscious control. When estrogen dips, your sympathetic nervous system (fight-or-flight) can become more active, triggering palpitations.
How common: Very. One study published in Menopause journal found that palpitations are reported by up to 40% of perimenopausal women. They are usually benign — but they are frightening.
Blood Pressure Changes
Some women notice their blood pressure creeping up during perimenopause — even with no prior history of hypertension.
What's happening: Estrogen helps keep blood vessels flexible and supports nitric oxide production (which dilates vessels). As estrogen declines, vascular stiffness increases and blood pressure may rise. This effect can be amplified by cortisol reactivity and sleep disruption.
Why Cardiovascular Risk Shifts During Perimenopause
This is the long-term consideration that deserves attention:
Before menopause, women have lower cardiovascular risk than men of the same age — partly due to estrogen's protective effects on cholesterol, blood vessel health, and inflammation
During and after the menopausal transition, this protective gap narrows
LDL cholesterol tends to rise, HDL may decrease, and inflammatory markers increase
Heart disease is the leading cause of death in women — and the risk transition begins during perimenopause, not after
When to Take Heart Symptoms Seriously
Palpitations during perimenopause are usually benign. But always consult a doctor if:
Palpitations are accompanied by chest pain, shortness of breath, or fainting
They are sustained (lasting minutes, not seconds)
They are increasing in frequency or severity
You have a family history of heart disease or arrhythmia
You have other cardiac risk factors (hypertension, diabetes, smoking, obesity)
The message: Don't dismiss heart symptoms as "just perimenopause" without appropriate evaluation. And don't let a doctor dismiss them as "just anxiety" without a cardiac workup.
Your Musculoskeletal System
Estrogen's role: Estrogen has anti-inflammatory properties, supports joint cartilage and synovial fluid production, maintains bone density through osteoblast activity, and influences muscle repair and strength.
Joint Pain and Morning Stiffness
What it feels like:
Waking up with stiff fingers, hips, or shoulders that take a while to loosen
New aching in joints that never bothered you before — especially hands, knees, hips
A general sense of stiffness that wasn't there a year ago
Joint symptoms that worsen before your period (when estrogen drops)
What's happening: Estrogen has anti-inflammatory effects on joint tissue and helps maintain the synovial fluid that lubricates your joints. As estrogen fluctuates and declines, inflammation increases and joint lubrication decreases. Research published in Maturitas found that musculoskeletal symptoms are among the most commonly reported during the menopausal transition — yet they're among the least recognized as hormonal.
The diagnostic trap: Many women see a rheumatologist who runs autoimmune panels (RA, lupus), finds nothing, and says "you're fine." The joint pain is real — it's just hormonal, not autoimmune (though both can coexist).
Muscle Tension, Aches, and Weakness
Beyond joints, perimenopause affects muscles:
Increased muscle tension — especially neck, shoulders, and jaw (some women develop TMJ symptoms)
Slower recovery after exercise
Reduced muscle mass (sarcopenia begins accelerating)
A general feeling of physical fragility — your body doesn't bounce back like it used to
What's happening: Estrogen and testosterone both support muscle protein synthesis. As both decline, maintaining muscle mass requires more intentional effort — particularly adequate protein (1.2–1.6 g/kg/day) and resistance training.
Bone Density — The Silent Change You Can't Feel
You can't feel bone density declining. There are no symptoms — until a fracture occurs.
What's happening: Estrogen directly supports osteoblasts (the cells that build new bone). During and after perimenopause, bone resorption begins to outpace bone formation. The most rapid bone loss occurs in the first 5–7 years after menopause, but the process begins during perimenopause.
What to do now:
Ensure adequate calcium (1,200 mg/day from food + supplements if needed)
Optimize vitamin D (test your levels; many women are deficient)
Prioritize weight-bearing and resistance exercise
Discuss bone density screening (DEXA scan) with your provider around menopause
Frozen Shoulder and Other Surprising Connections
Adhesive capsulitis (frozen shoulder) peaks in women aged 40–60 — and emerging research suggests a hormonal connection. Women in perimenopause and early postmenopause are disproportionately affected.
Other musculoskeletal surprises linked to hormonal changes:
Carpal tunnel syndrome — worsening or new onset
Trigger finger
Plantar fasciitis
Tendon stiffness and reduced flexibility
If you've developed any of these in your 40s and have no clear mechanical cause, hormones may be a contributing factor.
Your Thermoregulatory System
Estrogen's role: Estrogen helps regulate the hypothalamus — the brain's thermostat. It keeps the "thermoneutral zone" (the temperature range your body considers comfortable) wide and stable.
Hot Flashes — What's Actually Happening Inside
What it feels like:
A sudden, intense wave of heat — usually beginning in the chest, rising to the neck and face
Skin reddening and visible flushing
Profuse sweating — sometimes followed immediately by chills
Duration: typically 1–5 minutes, but can feel much longer
Frequency: from occasional to 20+ per day in severe cases
What's happening: Fluctuating estrogen narrows your thermoneutral zone — the range of body temperature your hypothalamus considers "normal." Instead of tolerating a range of, say, 2°C, your zone may shrink to 0.5°C. Even a tiny temperature increase triggers a full cooling response: vasodilation (blood rushes to the skin surface), sweating, and elevated heart rate.
Your body isn't overheating. Your thermostat has become hypersensitive.
Night Sweats and Temperature Dysregulation
Night sweats are hot flashes that occur during sleep — but they feel different because:
You're horizontal and covered — trapping heat
You wake mid-episode, often disoriented
The sweating can be drenching — soaking through pajamas and sheets
Cortisol spikes in response, making it nearly impossible to fall back asleep
The chills that follow add another layer of sleep disruption
Cold Flashes and Chills — The Symptom Nobody Mentions
Less discussed but very real: some women experience cold flashes — sudden episodes of intense cold or shivering, sometimes alternating with hot flashes.
What's happening: The same thermoregulatory instability that causes hot flashes can also trigger inappropriate cooling responses — vasoconstriction and shivering when you're not actually cold.
If you've been Googling "sudden chills perimenopause" and found nothing — you're not alone, and it's real.
Your Digestive System
Estrogen's role: Estrogen influences gut motility (how fast food moves through your system), gut barrier integrity, bile production, microbiome composition, and inflammatory tone in the GI tract.
Bloating, Gas, and the Perimenopause Gut
What it feels like:
Persistent bloating — especially after meals
Increased gas (sometimes embarrassingly so)
A feeling of abdominal distension that worsens through the day
Clothes fitting differently around the midsection — not from fat, from bloat
What's happening: Estrogen fluctuations affect gut motility and water retention. Progesterone decline can slow intestinal transit. Cortisol reactivity affects the gut-brain axis. And the gut microbiome itself is shifting — which brings us to the estrobolome.
Altered Bowel Habits — Constipation, Urgency, or Both
Some women develop constipation. Others experience urgency or looser stools. Many alternate between both.
What's happening: Estrogen and progesterone both influence smooth muscle contractions in the intestinal wall. Fluctuating levels create inconsistent motility. Stress hormones compound the effect. And if your gut microbiome is disrupted (by poor diet, stress, or medications), the instability is amplified.
Pattern: Many women notice digestive symptoms correlate with their cycle phase — suggesting a direct hormonal link.
Nausea and Appetite Changes
Less commonly discussed:
Waves of nausea — sometimes reminiscent of early pregnancy
Appetite fluctuations — intense hunger one day, no appetite the next
New food sensitivities — foods you always tolerated now cause discomfort
These shifts are related to estrogen's influence on gastric acid production, bile flow, and the gut-brain axis.
The Estrobolome — How Your Gut Metabolizes Hormones
Your gut contains a specialized collection of bacteria called the estrobolome — microbes that produce an enzyme (beta-glucuronidase) that influences how much estrogen is recycled or eliminated by your body.
A healthy, diverse microbiome → efficient estrogen metabolism → better hormonal balance
A disrupted microbiome → impaired estrogen clearance → potential estrogen dominance symptoms (heavier periods, breast tenderness, bloating)
Supporting your estrobolome:
High-fiber diet (25–35g/day)
Diverse plant foods (aim for 30+ plant species per week)
Fermented foods (yogurt, kefir, sauerkraut, kimchi)
Prebiotic foods (garlic, onions, leeks, asparagus)
Minimizing ultra-processed foods and unnecessary antibiotics
Your Skin, Hair, and Nails
Estrogen's role: Estrogen supports collagen production, skin hydration (via hyaluronic acid), sebum regulation, hair follicle cycling, and nail keratin structure.
Dry, Thinning, or Itchy Skin
What it feels like:
Skin that feels drier and duller — especially on the face, arms, and shins
A loss of "plumpness" or elasticity
Itching (formication) — sometimes a crawling sensation on the skin
Skin that seems to wrinkle or crease more easily
What's happening: Estrogen stimulates collagen and hyaluronic acid production. Studies show that women lose approximately 30% of their skin collagen in the first five years of menopause. This process begins during perimenopause. Skin becomes thinner, drier, and less elastic.
Acne That Returns After Decades
What it feels like:
Breakouts on the chin, jawline, and lower cheeks — areas associated with hormonal acne
Cystic, painful spots that are different from teenage acne
Acne appearing alongside dry skin — the confusing combination of oily and dry
What's happening: As estrogen declines, the relative influence of androgens (like testosterone) increases — even though testosterone itself is also declining. This relative androgen dominance stimulates sebaceous glands, particularly in hormone-sensitive areas of the face.
Hair Thinning on Your Head — Hair Growth Where You Don't Want It
What it feels like:
Hair that seems thinner, less voluminous, or falls out more in the shower
Widening part line or visible scalp
Simultaneously: new or coarser hair on the chin, upper lip, or cheeks
What's happening: The same relative androgen shift that causes adult acne affects hair follicles. Estrogen supports the growth phase (anagen) of head hair — as it declines, hair spends less time growing and more time resting and shedding. Conversely, androgens stimulate vellus-to-terminal hair conversion on the face and body.
Brittle Nails and Texture Changes
Nails that split, peel, or break more easily
Ridges (horizontal or vertical) that weren't there before
Slower nail growth
What's happening: Estrogen supports keratin production and nail bed hydration. As levels decline, nail structure and growth rate are affected.
What's Driving These Changes — Estrogen, Collagen, and Androgens
All skin, hair, and nail changes in perimenopause trace back to three intersecting shifts:
Declining estrogen → less collagen, less hydration, thinner skin
Relative androgen dominance → acne, facial hair, scalp hair changes
Reduced microcirculation → less nutrient delivery to skin and hair follicles
Your Urinary and Pelvic System
Estrogen's role: Estrogen maintains the health, thickness, and elasticity of the vaginal and urethral tissues, supports the vaginal microbiome (lactobacilli), and contributes to pelvic floor muscle tone.
Urinary Urgency, Frequency, and Leaking
What it feels like:
Needing to urinate more often — including at night (nocturia)
A sense of urgency — needing to go now
Stress incontinence — leaking when you cough, sneeze, laugh, or exercise
Urge incontinence — leaking before you reach the bathroom
What's happening: The urethra and bladder lining are estrogen-dependent tissues. As estrogen declines, these tissues become thinner and less resilient, and the muscles around the urethra weaken.
Recurrent UTIs — The Hormonal Connection
If you've started getting UTIs more frequently — especially without obvious risk factors — hormones may be the reason.
What's happening: Estrogen supports the vaginal microbiome (particularly lactobacilli), which creates an acidic environment that protects against pathogens. As estrogen declines, vaginal pH rises, lactobacilli decrease, and pathogenic bacteria — including E. coli — can more easily colonize the vaginal and urethral area.
Evidence-based solution: Vaginal estrogen (cream, ring, or tablet) is highly effective at restoring tissue health, reducing UTI recurrence, and relieving urinary symptoms. It's localized (not systemic), has an excellent safety profile, and is appropriate for most women — including many who cannot take systemic HRT.
Vaginal Dryness and Changes in Comfort
What it feels like:
Dryness, irritation, or a feeling of thinness
Discomfort during intercourse — sometimes significant
Mild spotting or bleeding after sex
A general sense of fragility in vaginal tissue
What's happening: This is Genitourinary Syndrome of Menopause (GSM) — a progressive condition caused by sustained low estrogen. Unlike hot flashes (which often improve over time), GSM tends to worsen without treatment.
Critical point: GSM does not resolve on its own. And many women suffer in silence due to embarrassment. Effective treatments exist — vaginal estrogen, vaginal moisturizers, and hyaluronic acid-based products — and should be discussed openly with your provider.
Pelvic Floor Weakness
The pelvic floor — the hammock of muscles supporting your bladder, uterus, and rectum — is estrogen-sensitive. As estrogen declines:
Muscle tone decreases
Connective tissue becomes less elastic
Risk of prolapse (descent of pelvic organs) increases
What helps: Pelvic floor physiotherapy, Kegel exercises (done correctly — not just randomly), and in some cases, pessary devices or surgical options. Starting pelvic floor work during perimenopause — before significant weakening occurs — is the best prevention strategy.
Your Immune and Inflammatory System
Estrogen's role: Estrogen is a potent immunomodulator. It has anti-inflammatory properties and helps regulate the balance between different immune cell types. It also influences histamine release and allergic responses.
Why Inflammation Increases During Perimenopause
As estrogen's anti-inflammatory effects become less consistent:
Inflammatory markers (CRP, IL-6, TNF-α) can rise
Low-grade chronic inflammation — sometimes called "inflammaging" — increases
This contributes to joint pain, fatigue, brain fog, cardiovascular changes, and weight gain
The inflammatory shift is one of the unifying mechanisms that connects symptoms across multiple body systems.
Autoimmune Flares and New Sensitivities
Women with pre-existing autoimmune conditions (Hashimoto's thyroiditis, rheumatoid arthritis, lupus, MS) may experience flares during perimenopause — because estrogen fluctuations destabilize the immune system that these conditions depend on being regulated.
Some women also notice new sensitivities — to foods, chemicals, or environmental triggers — that they never had before.
Allergies, Histamine, and Hormonal Cross-Reactivity
This is an emerging area of research that many women are experiencing before science has fully caught up:
Histamine intolerance can worsen during perimenopause — because estrogen influences DAO (diamine oxidase), the enzyme that breaks down histamine
Symptoms: hives, flushing, nasal congestion, headaches, digestive upset — all worse around ovulation or before menstruation
Some women develop new allergies or notice existing allergies becoming more severe
Evidence level: This area is supported by growing but limited evidence. The estrogen-histamine connection is biologically plausible and clinically observed, but large-scale studies are still needed.
Your Metabolic and Endocrine System
Estrogen's role: Estrogen influences insulin sensitivity, fat distribution, leptin signaling (appetite regulation), and thyroid hormone metabolism.
Weight Redistribution — Why Your Shape Is Changing
What it feels like:
Weight gain — or weight redistribution — especially around the abdomen
Your clothes fit differently even if the scale hasn't changed dramatically
The strategies that always worked for weight management no longer produce results
What's happening: Declining estrogen shifts fat storage from a gynoid pattern (hips and thighs) to an android pattern (abdomen). This isn't just cosmetic — visceral abdominal fat is metabolically active and associated with increased cardiovascular and metabolic risk.
This shift occurs even without changes in caloric intake or exercise — it's a hormonal redistribution, not a behavioral failure.
Insulin Resistance and Blood Sugar Instability
Estrogen helps maintain insulin sensitivity — the ability of your cells to use glucose efficiently. As estrogen fluctuates:
Cells become less responsive to insulin
Blood sugar levels spike and crash more easily
This triggers cravings (especially for sugar and refined carbs), energy crashes, and increased cortisol release
The cortisol response further worsens insulin resistance — creating a self-reinforcing cycle
What helps: Prioritizing protein at every meal, choosing complex carbohydrates paired with fat and fiber, and reducing refined sugar and alcohol. The Peri Plate Method was designed specifically to address this cycle.
Thyroid Interactions — When Two Transitions Collide
Thyroid dysfunction becomes more common as women age — and perimenopause and thyroid changes can happen simultaneously, creating diagnostic confusion:
Key difference: Perimenopause typically causes hot flashes and temperature dysregulation upward (feeling too hot). Hypothyroidism typically causes cold intolerance (feeling too cold). But overlap is common, and both can coexist.
Action: Ask your provider for a complete thyroid panel (TSH, Free T4, Free T3, thyroid antibodies) — not just TSH alone.
Fatigue That Goes Beyond Tired
Perimenopausal fatigue is distinctive:
It's not proportional to activity — you can be exhausted after doing nothing
Rest doesn't fully resolve it — you sleep and still wake unrested
It feels cellular — like your battery can't hold a full charge
It fluctuates — some days are manageable, others are crushing
What's happening: Fatigue in perimenopause is multifactorial:
Disrupted sleep (from night sweats, insomnia, cortisol spikes)
Hormonal instability directly affecting energy regulation
Insulin resistance creating energy crashes
Inflammation consuming metabolic resources
Possible iron deficiency (from heavier periods)
Possible thyroid changes
If fatigue is your dominant symptom, it's worth investigating all potential contributors — not just hormones.
What Women Actually Experience — The Whole-Body Reality
"I Thought I Was Falling Apart"
"At 46, I had a list: brain fog, joint pain, palpitations, insomnia, digestive issues, dry skin, thinning hair, anxiety, and exhaustion. I was seeing five different specialists, none of whom talked to each other. My rheumatologist said my joints were fine. My cardiologist said my heart was fine. My dermatologist gave me topical creams. My GP suggested antidepressants. Nobody — not one person — said: 'Have you considered that all of these symptoms might be connected to perimenopause?' I found that answer on my own, online, at 2 a.m. And I cried — not from sadness, but from relief."
"Every Specialist Saw One Piece — No One Saw the Whole Picture"
"The fragmentation of medical care is the biggest problem for women in perimenopause. Each doctor sees their organ system. Nobody sees the whole woman. When I finally saw a menopause specialist, she looked at my entire symptom list and said: 'These are all hormonal. All of them. Let's treat the root cause.' In one appointment, she did more than five specialists had done in two years."
"Understanding the Body Systems Changed How I Advocated for Myself"
"Once I understood that estrogen receptors were everywhere — in my brain, my gut, my joints, my skin — I stopped feeling like a hypochondriac. I started walking into appointments with a framework: 'Here are my symptoms, organized by body system. Here's why I believe they're connected to perimenopause. Here's what I'd like to explore.' That shift — from passive patient to informed advocate — changed everything."
The Master Symptom Map — Every System at a Glance
Print this table. Bring it to your next appointment. Show your doctor the full picture.
What to Do With This Information
How to Talk to Your Doctor Using the Body Systems Framework
This article isn't just educational — it's a communication tool.
When you walk into your doctor's office with a random list of 15 symptoms, it can feel (and look) overwhelming. But when you organize those same symptoms by body system, something shifts:
Instead of: "I have brain fog, joint pain, palpitations, bloating, dry skin, insomnia, anxiety, and hair loss — and I'm exhausted."
Try: "I'm experiencing symptoms across multiple body systems that I believe are connected to perimenopause. In my nervous system: brain fog and anxiety. Cardiovascular: palpitations. Musculoskeletal: joint pain. Digestive: bloating. Skin: dryness and hair changes. Sleep is disrupted. I've been tracking these for [X weeks]. Can we discuss whether hormonal changes might be the common driver?"
That second approach is harder to dismiss. It demonstrates knowledge, preparation, and pattern recognition. And it invites a conversation about root cause — not just symptom-by-symptom management.
Tracking Symptoms Across Systems
Track your symptoms daily using the body systems framework:
🔎 Resources That Help You Connect the Dots
This article may contain affiliate links. We only recommend products we've researched and believe may be genuinely useful for women navigating perimenopause. Affiliate commissions help support this site at no extra cost to you.
1. Balance App (by Dr. Louise Newson)
Best for: Free, medically informed symptom tracking across body systems — generates shareable health reports
Why it helps here: Tracks symptoms in multiple categories, revealing cross-system patterns over time. The generated report is designed to facilitate medical conversations
Strengths: Free, comprehensive symptom categories, doctor report feature
Limitations: UK-developed; some healthcare pathway info less relevant in US
2. "The Menopause Manifesto" by Dr. Jen Gunter
Best for: Comprehensive, evidence-based understanding of how perimenopause and menopause affect every body system
Why it helps here: Organized by topic with rigorous science — covers cardiovascular, bone, brain, metabolic, and genitourinary health in detail
Strengths: Authoritative, myth-busting, thorough
Limitations: Dense for casual readers
3. "The New Menopause" by Dr. Mary Claire Haver
Best for: Practical protocols for addressing symptoms across body systems — especially nutrition, inflammation, and body composition
Why it helps here: Translates the science into action plans. Particularly strong on metabolic and inflammatory aspects
Strengths: Action-oriented, accessible, covers the Galveston Diet approach
Limitations: One clinical perspective — complement with individual guidance
4. Magnesium Glycinate (200–400 mg)
Best for: Cross-system support — sleep, anxiety, muscle tension, headaches, palpitations
Why it helps here: Magnesium is involved in hundreds of enzymatic processes across body systems. Many perimenopausal women are deficient. Glycinate form is the most bioavailable and gentle on the gut
Evidence level: Modest but positive for sleep and muscle relaxation. Low risk for most people
Look for: Third-party tested (USP or NSF certified)
Limitations: Not a substitute for medical treatment. Discuss with provider if taking medications
5. Omega-3 Fish Oil (EPA/DHA — 1,000–2,000 mg)
Best for: Anti-inflammatory support across joints, cardiovascular system, brain, and skin
Why it helps here: EPA and DHA omega-3 fatty acids are the most potent dietary anti-inflammatory compounds. During perimenopause, when systemic inflammation rises, omega-3 supplementation may support multiple body systems simultaneously
Evidence level: Strong for cardiovascular benefit and anti-inflammatory effects. Moderate for joint pain and mood support. Modest for skin health
Look for: Triglyceride form, third-party tested for purity (IFOS certified), minimum 1,000 mg combined EPA+DHA
Limitations: Results take 4–8 weeks. Quality varies enormously. May interact with blood-thinning medications
YMYL disclosure: No supplement replaces a comprehensive medical evaluation or treatment plan. These products may offer supportive benefits alongside — not instead of — professional medical care. Individual results vary. Always consult your healthcare provider before starting new supplements, especially if you have existing conditions or take medications.
Your Body Isn't Failing — It's Recalibrating
If you've read this entire article, you now know something that many healthcare providers don't adequately explain:
Perimenopause is a whole-body experience.
It's not "just periods and hot flashes." It's your brain, your heart, your joints, your gut, your skin, your bladder, your immune system, your metabolism — all responding to the same hormonal shift.
And that knowledge changes everything. Because:
When you understand why your joints ache, you stop worrying about arthritis and start addressing inflammation.
When you understand why your heart races, you stop panicking about cardiac disease and start managing your nervous system.
When you understand why your gut is unpredictable, you stop cycling through elimination diets and start supporting your estrobolome.
When you see all the systems on one page, you stop feeling like a hypochondriac and start recognizing a pattern with a name and a cause.
Your body isn't falling apart. It's going through the most significant hormonal recalibration since puberty. And just like puberty, it's temporary — even when it doesn't feel like it.
You're not broken. You're in transition. And now you have the map.
FAQ — Physical Symptoms of Perimenopause
Q: Can perimenopause cause joint pain?
A: Yes. Estrogen has anti-inflammatory properties and supports joint lubrication. As estrogen fluctuates during perimenopause, joint pain and morning stiffness are very common — especially in hands, hips, and shoulders. This is often misdiagnosed as early arthritis.
Q: Why does perimenopause affect so many body systems?
A: Estrogen receptors exist in nearly every tissue — brain, heart, bones, gut, skin, bladder, and immune system. When estrogen fluctuates during perimenopause, all these systems are affected simultaneously, producing wide-ranging symptoms.
Q: Can perimenopause cause digestive problems?
A: Yes. Estrogen influences gut motility, microbiome composition, and gut barrier integrity. Bloating, altered bowel habits, nausea, and increased gas are common during perimenopause and are directly linked to hormonal fluctuations.
Q: Are heart palpitations normal during perimenopause?
A: Heart palpitations are reported by up to 40% of perimenopausal women and are usually benign, caused by estrogen's effect on the autonomic nervous system. However, new palpitations should always be evaluated by a doctor to rule out cardiac causes.
Q: Does perimenopause cause skin changes?
A: Yes. Estrogen supports collagen production, skin hydration, and elasticity. During perimenopause, skin may become drier, thinner, and less elastic. Some women also develop hormonal acne due to the relative increase in androgen influence.
Q: Can perimenopause cause allergies or histamine issues?
A: Emerging evidence suggests that estrogen fluctuations can worsen histamine intolerance by affecting DAO, the enzyme that breaks down histamine. Some women develop new allergies or sensitivities during perimenopause, though research in this area is still growing.
Ready to take the next step?
(https://perimenopausecompass.com/free-14-day-tracker) to find your personal triggers.
Get the Perimenopause Nutrition Protocol to support your nervous system from the inside out.
Visit our (https://perimenopausecompass.com/start-here) page for more foundational guidance.
Get the Perimenopause Nutrition Protocol ($29 + bonus) → https://perimenopausecompass.gumroad.com/l/iecoc
______________________________________
Disclaimer Education only — not medical advice. Consult a qualified healthcare professional for diagnosis and treatment.
Sources / References


After 4–8 weeks, review:
Which systems are most affected?
Do symptoms cluster at certain cycle points?
Are certain systems improving or worsening?
What triggers seem to amplify symptoms across systems?
This data is clinically powerful — and personally validating.
Perimenopause Compass
Contact
hello@perimenopausecompass.com
© 2026 All rights reserved.
