Perimenopause vs Menopause vs Premenopause: Clear Guide
Confused by perimenopause vs menopause vs premenopause? This clear guide explains the real differences — what happens in each stage, which one you're in, and what to do next.
Perimenopause Compasss
2/14/202616 min read
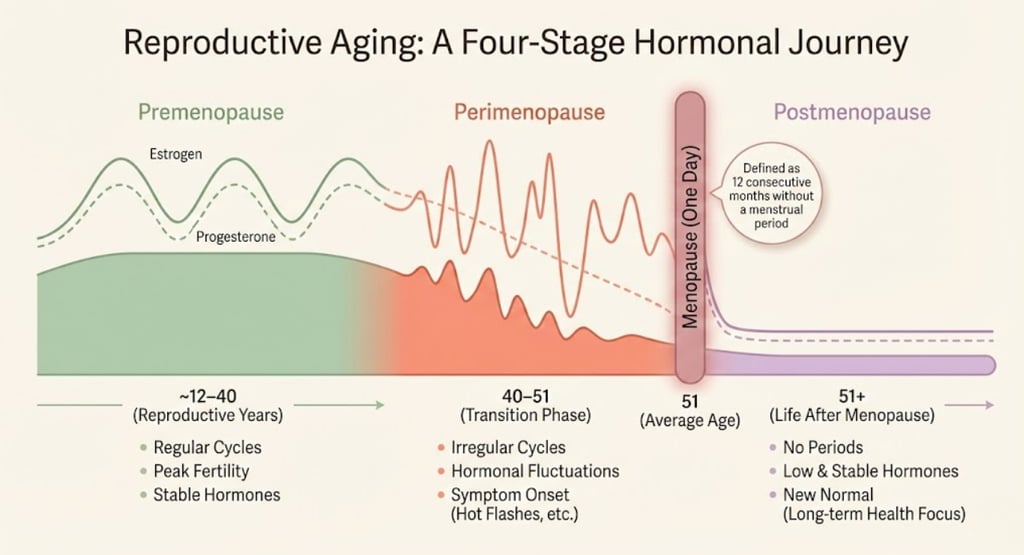
Premenopause. Perimenopause. Menopause. Postmenopause.
Four words that sound almost identical, get used interchangeably by doctors, media, and friends — and leave millions of women with absolutely no idea which stage they're actually in.
If you've ever Googled "am I in perimenopause or menopause?" or "what's the difference between premenopause and perimenopause?" — you're not confused because you're uninformed. You're confused because the terminology is genuinely confusing, and almost no one explains it clearly.
This article fixes that. No medical jargon. No vague definitions. Just a clear, comprehensive comparison of every stage — what each one means, what happens in your body, what it feels like, and most importantly, how to figure out where you are right now.
Why These Terms Are So Confusing — And Why It Matters
The Terminology Problem No One Fixes
Here's the core issue: the word "menopause" is used to describe at least three different things, and people rarely specify which one they mean.
When someone says "menopause," they might mean:
The event — the specific day that marks 12 months since your last period (the clinical definition)
The symptoms — hot flashes, night sweats, mood changes (which are actually perimenopause symptoms in most cases)
The life stage — the general era of midlife hormonal change (which spans perimenopause, menopause, and postmenopause combined)
This isn't just a semantic problem. It creates real clinical confusion:
Women experiencing perimenopause symptoms are told they're "going through menopause" — and then wonder why they still have periods
Women who've reached menopause are told their symptoms should be over — but they're still having hot flashes (which is normal in postmenopause)
Women in their early 40s are told they're "too young for menopause" — when what they're experiencing is perimenopause, which can start a decade before menopause
What's at Stake When You Don't Know Which Stage You're In
This isn't just about vocabulary. Your stage determines your care.
Treatment options differ — hormone therapy guidelines, for example, are specifically designed around where you are in the transition
Testing recommendations vary — blood tests are unreliable in perimenopause but more useful in postmenopause
Health screening changes — bone density, cardiovascular risk, and cancer screening recommendations shift at each stage
Self-understanding matters — knowing that your symptoms are perimenopause (a temporary transition) rather than menopause (a permanent state) fundamentally changes how you relate to your experience
Getting the terminology right isn't pedantic. It's empowering.
The Quick Comparison — All Three Stages at a Glance
Premenopause vs Perimenopause vs Menopause — Summary Table
Let's get the overview on the table first. The detail comes after.
The One Sentence That Explains It All
If you need a single sentence to understand the entire picture, here it is:
Premenopause is your "before." Perimenopause is the bumpy transition. Menopause is the one-day finish line. And postmenopause is everything after.
Most of what people experience — the symptoms, the struggles, the changes — happens during perimenopause, not menopause itself. Menopause is just the milestone that confirms the transition is complete.
What Is Premenopause?
Definition and Hormonal Profile
Premenopause refers to your entire reproductive life before any menopausal transition begins. It's the years when your ovaries, hormones, and menstrual cycle function in their normal, reproductive pattern.
Hormonally, premenopause looks like this:
Estrogen and progesterone cycle predictably each month
Ovulation occurs consistently (typically every 21–35 days)
FSH (Follicle-Stimulating Hormone) stays within a normal, low range
Fertility is at its peak (though it gradually declines after the early 30s)
For most women, premenopause spans from their first period (around age 12–13) to their early-to-mid 40s — roughly 25 to 35 years.
What Premenopause Feels Like
In premenopause, your hormonal experience is what you're used to. It's your baseline — the "normal" against which everything else gets compared.
That doesn't mean premenopause is symptom-free. You may experience:
Normal PMS (bloating, mood shifts, breast tenderness)
Menstrual cramps
Hormonal acne around your period
Variations in energy and mood across your cycle
But these experiences are cyclical, predictable, and consistent. They don't escalate. They don't disrupt your sleep for weeks. They don't make you feel like a different person.
When those things start happening — when your baseline shifts — that's the signal that premenopause is ending and perimenopause is beginning.
When Premenopause Ends and Perimenopause Begins
There is no blood test, no scan, and no definitive moment that marks the transition from premenopause to perimenopause. It's a gradual shift, not a switch.
The earliest signs that you may be moving from premenopause into perimenopause include:
Cycles becoming slightly shorter (e.g., 25 days instead of 28–30)
PMS intensifying — or appearing for the first time
Sleep quality shifting — not dramatically, but noticeably
New anxiety or mood changes that feel different from your usual pattern
A gut feeling that something hormonal has changed
These signs can appear years before periods become visibly irregular. That's why so many women don't realize they've entered perimenopause until they're well into it.
What Is Perimenopause?
Definition and Hormonal Profile
Perimenopause is the transitional phase when your ovaries gradually produce less estrogen and progesterone, ovulation becomes inconsistent, and your body moves toward the end of its reproductive function.
"Peri" means "around" — so perimenopause literally means "around menopause." It's the process of getting there.
Hormonally, perimenopause is characterized by instability, not just decline:
Estrogen doesn't simply drop — it fluctuates wildly, sometimes spiking to levels higher than your peak reproductive years, then crashing. These unpredictable swings are what drive most acute symptoms.
Progesterone declines more steadily — because it's only produced after ovulation, and ovulation is becoming less consistent. This often happens before estrogen changes become obvious.
FSH rises as your pituitary gland tries harder to stimulate aging ovaries — but it's highly variable day-to-day, which is why single blood tests are unreliable.
Testosterone gradually decreases — contributing to changes in energy, libido, and muscle mass.
The key insight: perimenopause is hormonal chaos, not hormonal absence. Your levels aren't just low — they're unpredictable. And that unpredictability is what makes symptoms come and go, shift in intensity, and feel so confusing.
When It Starts — And Why It's Earlier Than You Think
Most women expect menopause-related changes in their early 50s. But perimenopause typically begins much earlier:
Average onset: Mid-40s (around 44–46)
Early-normal onset: Late 30s to early 40s (38–43)
Average duration: 4–8 years
Possible duration: 2–12+ years
This means a woman who reaches menopause at the average age of 51 may have entered perimenopause at 43 or even earlier — years before she would have suspected it.
And because early perimenopause symptoms are subtle — slightly shorter cycles, worse PMS, sleep changes, new anxiety — most women spend months or years attributing them to stress, aging, or burnout rather than recognizing the hormonal shift.
The Two Sub-Stages of Perimenopause (STRAW+10)
The internationally recognized STRAW+10 classification divides perimenopause into two sub-stages:
Get the Perimenopause Nutrition Protocol ($29 + bonus)
Get the Perimenopause Nutrition Protocol ($29 + bonus)


This distinction matters because the treatment conversation changes between early and late perimenopause. Understanding which sub-stage you're in helps you and your doctor make more informed decisions.
What Perimenopause Actually Feels Like
Perimenopause is the stage that produces the vast majority of what people colloquially call "menopause symptoms." The experience varies enormously from woman to woman, but commonly includes:
Vasomotor symptoms:
Hot flashes — sudden waves of intense heat, often in the chest, neck, and face
Night sweats — ranging from mild dampness to soaking through pajamas and sheets
Flushing and sudden warmth during the day
Mood and cognitive symptoms:
New or intensified anxiety — including physical anxiety (chest tightness, racing heart)
Irritability, rage, or emotional overwhelm
Brain fog — difficulty concentrating, word-finding problems, memory lapses
Mood swings that feel disproportionate or unpredictable
Depressive symptoms — sadness, flatness, or loss of motivation
Sleep disruption:
Difficulty falling asleep
Waking at 3–4 a.m. and unable to return to sleep
Light, fragmented, or unrefreshing sleep
Physical symptoms:
Joint pain and morning stiffness
Heart palpitations
Fatigue that rest doesn't fix
Weight redistribution — especially around the abdomen
Changes in libido and vaginal moisture
Headaches or migraines (new or worsening)
Hair, skin, and nail changes
Urinary changes — frequency, urgency
Menstrual changes:
Shorter cycles → longer cycles → skipped cycles
Heavier or lighter flow than usual
Unpredictable timing
Worsening PMS
The critical thing to understand: these are perimenopause symptoms, not menopause symptoms. If you're experiencing these and still having periods (however irregular), you're in perimenopause — even if everyone around you calls it "menopause."
What Is Menopause?
Definition — It's One Day, Not a Phase
This is the biggest misconception in women's health terminology:
Menopause is not a phase. It's a single point in time.
Specifically, menopause is defined as the day that marks exactly 12 consecutive months since your last menstrual period. The average age is 51 in the US and UK, though the normal range spans from approximately 45 to 58.
You can only identify menopause retrospectively — you don't know your last period was your last period until a full year has passed without another one.
This means:
If you haven't had a period in 10 months, you're in late perimenopause, not menopause yet
If you go 11 months without a period and then have one, the clock resets
The day you hit 12 months is technically your menopause date — but nothing dramatic happens on that specific day
The Difference Between Menopause and Postmenopause
This is where the terminology gets most confused:
Menopause = the milestone (one day)
Postmenopause = everything after that day (the rest of your life)
When people say "I'm going through menopause" and they mean they're experiencing hot flashes and mood changes, they almost always mean either perimenopause (if they still have periods) or postmenopause (if periods have stopped for 12+ months).
Menopause itself — the event — has no symptoms. It's simply the confirmation that your ovaries have stopped releasing eggs and your reproductive years are complete.
What Changes After Menopause
When menopause is confirmed, several things shift:
Hormonally:
Estrogen stabilizes at a consistently low level — the wild fluctuations of perimenopause are over
Progesterone remains minimal
FSH stabilizes at a high level
The hormonal chaos calms — and with it, many (but not all) symptoms begin to ease
Medically:
Pregnancy is no longer possible (contraception is no longer needed)
Hormone therapy guidelines shift — different risk-benefit calculations apply
Bone density decline accelerates — the first 5–7 years after menopause carry the highest bone loss risk
Cardiovascular risk increases — estrogen's heart-protective effects diminish
Vaginal and urinary health requires ongoing attention — these symptoms don't resolve on their own and often worsen without treatment
Experientially:
Many women feel a gradual easing — hot flashes become less frequent, sleep improves, mood stabilizes
Some women describe a sense of relief, clarity, or renewed energy once the hormonal storm passes
Others experience continued symptoms well into postmenopause — the SWAN study found that vasomotor symptoms last a median of 7.4 years total, often extending years beyond menopause
What Is Postmenopause? (The Stage Most Guides Leave Out)
Definition and Hormonal Profile
Postmenopause begins the day after menopause — and lasts for the rest of your life. It is the longest reproductive stage most women will experience.
Hormonally, postmenopause is characterized by stability at a new, lower baseline:
Estrogen: low and stable (primarily estrone, produced by fat tissue, rather than estradiol, produced by ovaries)
Progesterone: minimal
FSH: elevated but stable
Testosterone: continues its gradual age-related decline
The dramatic fluctuations of perimenopause are over. Your body has recalibrated to its new hormonal reality.
What Continues, What Improves, What's New
What typically IMPROVES in postmenopause:
Hot flashes and night sweats — decrease in frequency and intensity for most women (though some continue for years)
Mood volatility — the emotional roller coaster tends to stabilize
Brain fog — many women report cognitive clarity returning
Sleep — often improves, though postmenopausal sleep may differ from pre-perimenopausal sleep
What typically PERSISTS or EMERGES:
Vaginal dryness and atrophy (Genitourinary Syndrome of Menopause/GSM) — this is driven by sustained low estrogen and often worsens over time without treatment. Local estrogen therapy is safe and effective for most women
Urinary symptoms — increased urgency, frequency, and susceptibility to UTIs
Bone density loss — the most rapid decline occurs in the first 5–7 years after menopause
Cardiovascular changes — risk of heart disease increases; lipid profiles may shift
Skin and hair changes — ongoing effects of lower estrogen and collagen decline
Body composition shifts — maintaining muscle mass requires more intentional effort
What's sometimes NEW:
A sense of hormonal peace — the volatility is over
Renewed energy or motivation — some women describe postmenopause as a "new chapter"
An opportunity for proactive health optimization — bone health, heart health, pelvic floor strength, cognitive health
In some cases, sexual liberation — freedom from pregnancy concerns and, for some women, a renewed sense of desire
Postmenopause isn't a decline — it's a new physiological chapter. And with appropriate care (including HRT if chosen, nutrition, exercise, and screening), it can be a long and vital one.
Side-by-Side Comparison — Symptoms at Every Stage
Premenopause Symptoms vs Perimenopause Symptoms
Perimenopause Symptoms vs Menopause/Postmenopause Symptoms
The Master Comparison Table
What Women Actually Experience — When the Lines Blur
Medical tables are clean and organized. Real life is not. Here's what the intersection of these stages actually sounds like:
"I Don't Know Which Stage I'm In"
"I'm 47. My periods still come — but they're all over the place. Some months I skip, some months they're on time. I had a hot flash last week but not this week. My doctor says I'm 'probably perimenopausal' but hasn't really explained what that means versus menopause. Am I going through menopause? I genuinely don't know the answer, and I've been dealing with this for three years."
What's actually happening: This woman is in perimenopause — specifically, likely in the late menopausal transition (STRAW Stage -1). She has not reached menopause because she's still having periods. The confusion stems from the common misuse of "menopause" to describe what is actually the perimenopausal transition.
"My Doctor Uses These Words Interchangeably"
"When I described my symptoms at 44, my GP said I was 'entering menopause.' At 46, when I asked about HRT, a different doctor said I was 'premenopausal' because my blood test was normal. At 48, another doctor said I was 'menopausal.' I was still getting occasional periods. Three doctors, three different terms, none of them explained what they meant. I left every appointment more confused than when I arrived."
What's actually happening: Inconsistent medical terminology created three years of diagnostic confusion. This woman was in perimenopause throughout — but different providers used "menopause," "premenopause," and "menopausal" loosely. This is unfortunately common, and it's why patient education matters so much.
"I Thought Menopause Was the Hard Part — It Was Perimenopause All Along"
"For years, I dreaded 'menopause.' I thought that was when the symptoms would hit. By the time I actually reached menopause at 52 — 12 months without a period — I felt... better. Not perfect, but calmer. Stabler. The worst years were 46 to 51, during perimenopause. Nobody told me the transition would be harder than the destination. If I'd known that, I would have sought help sooner instead of waiting for some imaginary 'menopause' to deal with."
What's actually happening: This is one of the most common — and most costly — misunderstandings. The assumption that "menopause" is the hard part leads women to delay seeking help during perimenopause, enduring years of manageable symptoms because they think the "real thing" hasn't started yet.
What Science Says — How Doctors Classify the Stages
The STRAW+10 System Explained Simply
The Stages of Reproductive Aging Workshop (STRAW+10) is the internationally recognized scientific framework for classifying where a woman is in her reproductive timeline. Updated in 2012 by an international panel, it's the gold standard used by researchers and menopause specialists worldwide.
Here's how STRAW+10 maps the full reproductive lifespan:
FMP = Final Menstrual Period
What this system clarifies:
"Premenopause" in STRAW+10 corresponds to stages -5 through -3 (the reproductive years)
"Perimenopause" corresponds to stages -2 and -1 (the menopausal transition)
"Menopause" is stage 0 — a single retrospective point
"Postmenopause" covers stages +1a through +2 (everything after)
The beauty of this system is that it defines the stages by observable markers (cycle changes) rather than blood tests — because hormones are too variable during the transition to be reliable diagnostic tools.
Why the Medical Definition Matters for Your Care
Understanding which stage you're in isn't academic — it has practical medical implications:
What's Established vs. What's Still Being Refined
Scientifically established:
The STRAW+10 system is the accepted international standard for staging reproductive aging
Perimenopause is a distinct phase from menopause and postmenopause — with different hormonal profiles and clinical considerations
Symptom severity typically peaks in the late menopausal transition (Stage -1) — the 1–2 years surrounding the final menstrual period
Clinical diagnosis (symptoms + cycle changes + age) is more reliable than hormonal blood tests during the transition
Probable (growing evidence):
The transition stages may have more sub-phases than STRAW+10 currently captures — particularly within early perimenopause
Inflammatory markers and gut microbiome profiles may eventually help refine staging
Racial and ethnic differences in transition timing and experience may warrant population-specific modifications to staging criteria
Still debated:
Whether additional biomarkers (AMH, inhibin B) should be incorporated into routine staging
How to classify women whose transition is masked by hormonal contraception, hysterectomy, or IUD use
Whether a simpler, patient-facing classification system would improve self-recognition and earlier care-seeking
This article is for educational purposes and does not replace medical advice. If you're unsure which stage you're in, or if symptoms are affecting your quality of life, consult a healthcare provider — ideally one with menopause-specific training.
How to Figure Out Which Stage You're In Right Now
A Simple Self-Assessment by Age and Symptoms
While you can't diagnose your exact STRAW stage at home, you can estimate where you are based on three factors: your age, your cycle, and your symptoms.
You're likely still in PREMENOPAUSE if:
☐ You're under 40
☐ Your periods are regular and predictable (within 1–3 days of your usual)
☐ Your PMS is consistent and hasn't changed significantly
☐ You have no new symptoms that feel different from your usual baseline
☐ You have no family history of early menopause
You're likely in EARLY PERIMENOPAUSE if:
☐ You're between 38 and 47
☐ Your cycles have shortened slightly (e.g., 25 days instead of 28–30) or become slightly less predictable
☐ PMS has intensified or changed in character
☐ You've noticed new sleep disruption, anxiety, brain fog, or fatigue
☐ You haven't skipped a period yet, but something feels different
You're likely in LATE PERIMENOPAUSE if:
☐ You're between 44 and 53
☐ Your cycles vary significantly month to month — or you've started skipping periods
☐ You've had at least one gap of 60+ days between periods
☐ Hot flashes or night sweats have emerged
☐ Multiple symptoms are affecting your daily life
You've likely reached MENOPAUSE / entered POSTMENOPAUSE if:
☐ You're typically 49+ (but range is 45–58)
☐ It has been 12 consecutive months since your last period
☐ Symptoms may be stabilizing — or continuing but changing in character
☐ Your doctor has confirmed postmenopausal status (if tested, FSH is consistently elevated)
⚠️ Note: If you've had a hysterectomy (with ovary preservation), use a hormonal IUD, or have had endometrial ablation, you've lost the menstrual cycle marker. In these cases, symptom tracking and (sometimes) hormonal testing can help estimate your stage — work with a knowledgeable provider.
Why Blood Tests Won't Give You a Clear Answer
This bears repeating because it causes so much confusion:
During perimenopause, hormone blood tests are unreliable.
FSH fluctuates day to day — it can be "normal" today and elevated tomorrow
Estradiol swings wildly — a single measurement captures a moment, not a pattern
A "normal" result doesn't rule out perimenopause — and an "abnormal" result doesn't confirm it on its own
Blood tests become more useful after menopause, when hormones stabilize at their new baseline. But during the transition itself, your symptoms and cycle history are more diagnostically useful than your lab panel.
UK NICE guidelines explicitly state that in women over 45, blood tests are not required to diagnose perimenopause — clinical assessment is sufficient.
What to Ask Your Doctor
If you want clarity on your stage, come to your appointment prepared:
Bring your menstrual cycle history — dates and any changes over the past 6–12 months
Bring a symptom list — what you're experiencing, when it started, how it affects your life
Ask directly: "Based on my age, symptoms, and cycle changes, which stage of the transition do you think I'm in — early perimenopause, late perimenopause, or postmenopause?"
If your doctor seems uncertain, ask: "Would you recommend I see a menopause specialist?"
If blood tests are ordered, ask: "How will you interpret these results given that hormone levels fluctuate during perimenopause?"
Tools That Help You Understand Where You Are
🔎 Our Recommended Resources
This article may contain affiliate links. We only recommend products we've researched and believe may be genuinely useful for women navigating this transition. Affiliate commissions help support this site at no extra cost to you.
1. Balance App (by Dr. Louise Newson)
Best for: Free symptom tracking that generates health reports showing your symptom pattern over time
Why it helps here: When you're trying to determine your stage, tracking symptoms over weeks reveals patterns that a single snapshot can't. Balance generates a report you can bring to your doctor
Strengths: Free, medically informed, helps bridge the gap between "I think something is happening" and a productive medical conversation
Limitations: UK-developed; some healthcare pathway information may not apply in US contexts
2. "The Menopause Manifesto" by Dr. Jen Gunter
Best for: The definitive evidence-based guide to understanding all stages of the menopausal transition
Why it helps here: Dr. Gunter devotes significant attention to terminology, staging, and debunking myths — exactly what you need when sorting through premenopause, perimenopause, and menopause confusion. Excellent science, accessible writing
Strengths: Rigorous, empowering, comprehensive, myth-busting
Limitations: Dense for casual readers; one clinical perspective
3. "The New Menopause" by Dr. Mary Claire Haver
Best for: Women who want practical action plans alongside medical education — particularly nutrition, body composition, and treatment navigation
Why it helps here: Explains how care strategies differ at each stage, helping you match your approach to your current phase
Strengths: Action-oriented, accessible, addresses the "what do I do now?" question at every stage
Limitations: One approach — complement with individual medical guidance
4. Oura Ring (Gen 3)
Best for: Objective biometric tracking — particularly temperature trends and sleep architecture changes that correlate with hormonal shifts
Why it helps here: Body temperature fluctuations and sleep disruption are stage-specific markers. Tracking them objectively over months provides data that complements subjective symptom tracking
Strengths: Objective data, temperature trend analysis, longitudinal tracking capability
Limitations: $299+ investment, subscription for full features, correlative not diagnostic
YMYL disclosure: No app, book, or tracking device replaces a medical evaluation. These tools are recommended to support your understanding and enhance your medical conversations — not to self-diagnose. Individual experiences vary. Always consult a healthcare provider for clinical guidance.
Why Understanding the Difference Changes Everything
It might seem like this is just a vocabulary lesson. It's not.
When you understand the difference between premenopause, perimenopause, menopause, and postmenopause, several things shift:
You stop waiting for the wrong thing. Many women endure years of perimenopause symptoms while waiting for "menopause" to arrive — because they believe that's when they'll need help. In reality, perimenopause is when help is most needed and most effective.
You stop being gaslit by vague terminology. When a doctor says "your blood work is normal, so it's not menopause," you can respond: "I understand — but could this be perimenopause? I know hormone tests are unreliable during the transition."
You advocate more effectively for yourself. Knowing your stage allows you to ask specific questions, request appropriate screening, and evaluate treatment recommendations against the correct clinical context.
You understand that this is temporary. Perimenopause — the hardest part for most women — is a transition, not a permanent state. It has an end. Understanding the phases helps you see where you are on the map and know that you're moving forward, even when it doesn't feel like it.
You connect with the right information. An article about "menopause nutrition" may not be relevant if you're in early perimenopause. A guide to "postmenopause bone health" isn't urgent if you're 42. Knowing your stage helps you filter the noise and focus on what matters for you right now.
Clarity is not a luxury. It's a necessity.
And now you have it.
FAQ — Perimenopause vs Menopause vs Premenopause
Q: What is the difference between perimenopause and menopause?
A: Perimenopause is the transition phase when hormones fluctuate and symptoms emerge — lasting an average of 4–8 years. Menopause is the single point in time marking 12 consecutive months without a period. Most "menopause symptoms" actually occur during perimenopause.
Q: Is premenopause the same as perimenopause?
A: No. Premenopause is your entire reproductive life before any menopausal transition begins — with regular cycles and stable hormones. Perimenopause is the active transition when hormones start fluctuating and symptoms emerge. They are distinct stages.
Q: What are the 3 stages of menopause?
A: The three commonly referenced stages are perimenopause (the transition), menopause (12 months without a period), and postmenopause (life after menopause). Premenopause (your reproductive years before any change) is sometimes included as a fourth stage.
Q: How do I know if I'm in perimenopause or menopause?
A: If you're still having periods — even irregular ones — you're in perimenopause. Menopause is only confirmed after 12 consecutive months without a period. If it's been over a year since your last period, you've reached menopause and are now in postmenopause.
Q: Can you be in perimenopause at 40?
A: Yes. Perimenopause typically begins in the mid-40s but can start as early as the late 30s or early 40s. This is considered normal and is not the same as premature menopause, which refers to menopause occurring before age 40.
Q: What comes after menopause?
A: Postmenopause — which lasts for the rest of your life. Hormones stabilize at lower levels. Many symptoms gradually improve, though vaginal dryness and bone density changes often require ongoing management. Postmenopause is a new chapter, not a decline.


Ready to take the next step?
(https://perimenopausecompass.com/free-14-day-tracker) to find your personal triggers.
Get the Perimenopause Nutrition Protocol to support your nervous system from the inside out.
Visit our (https://perimenopausecompass.com/start-here) page for more foundational guidance.
Get the Perimenopause Nutrition Protocol ($29 + bonus) → https://perimenopausecompass.gumroad.com/l/iecoc
______________________________________
Disclaimer Education only — not medical advice. Consult a qualified healthcare professional for diagnosis and treatment.
Sources / References
Perimenopause Compass
Contact
Newsletter
hello@perimenopausecompass.com
© 2026 All rights reserved.
