Perimenopause Bloating: Why It Happens & How to Ease It
Perimenopause bloating can feel relentless — but it's not random. Discover why hormonal shifts cause belly bloating, what makes it worse, and gentle strategies that actually help.
LIFESTYLE
3/30/202612 min read
Your jeans fit fine this morning. By mid-afternoon, you can barely button them.
Your belly feels tight, swollen, pressurized — like something inflated it from the inside. It's not just after a big meal. It happens after coffee. After salad. After seemingly nothing at all.
You've cut gluten. You've tried probiotics. You've spent anxious nights wondering if it's something more serious. And yet the bloating keeps coming back — unpredictable, uncomfortable, and deeply frustrating.
If this sounds familiar, here's what you need to hear: bloating is one of the most common — and least talked about — symptoms of perimenopause. It's not in your head. It's not because you're eating "wrong." And it's not a mystery once you understand what your hormones are doing.
This article explains why perimenopause bloating happens, what the science actually says, what real women experience, and — most importantly — what you can do to find genuine relief.
This article is based on current medical knowledge and real-life experiences, but does not replace medical advice. If you experience persistent, severe, or unexplained abdominal bloating, please consult a healthcare provider.
What Does Perimenopause Bloating Actually Feel Like?
Bloating during perimenopause isn't just "feeling a bit full." It's a specific, often intense physical sensation that goes well beyond normal digestive discomfort.
The Many Faces of Hormonal Bloating
Women in perimenopause typically describe one or more of these patterns:
Abdominal distension — your belly visibly expands, sometimes by several inches, over the course of a day
Pressure and tightness — a sensation of internal swelling, as if your abdomen is filled with air or fluid
Puffiness everywhere — not just the belly, but fingers, ankles, face, and breasts feel swollen
Trapped gas and discomfort — cramping, gurgling, or a feeling that gas can't move through normally
Fluctuating bloating — flat stomach in the morning, visibly distended by evening — then flat again the next morning
Bloating that mimics PMS but lasts longer — the familiar premenstrual puffiness, except now it lingers for days or weeks instead of resolving when your period starts
The emotional weight of this symptom is real, too. Many women describe feeling self-conscious, confused, and exhausted by the constant physical changes in how their body looks and feels from one hour to the next.
Bloating vs. Weight Gain — How to Tell the Difference
This is one of the most common questions women ask — and the confusion is completely understandable.
Bloating:
Comes and goes (often within the same day)
Feels like swelling or pressure
May be accompanied by gas or digestive discomfort
Your weight on the scale may fluctuate by 2–5 pounds within 24 hours
Relieved by passing gas, having a bowel movement, or overnight rest
Weight gain:
Is gradual and persistent
Doesn't fluctuate dramatically day-to-day
Often concentrates around the midsection during perimenopause
Doesn't resolve overnight
Many perimenopausal women experience both — bloating layered on top of gradual midlife body composition changes. Understanding which is which helps you respond appropriately instead of blaming yourself for something that isn't about willpower.
Why Does Perimenopause Cause Bloating?
The answer involves more systems than you might expect. Bloating during perimenopause isn't just a "stomach problem" — it's a whole-body hormonal event.
Estrogen, Progesterone, and Water Retention
Estrogen directly influences how your body handles fluid. When estrogen levels are high (which happens frequently during perimenopause, often in erratic surges before the overall decline), your body retains more water. This creates puffiness, abdominal fullness, and that "inflated" feeling.
Meanwhile, progesterone — which normally helps counterbalance estrogen's effects — drops earlier and more consistently during perimenopause. The result is a state of relative estrogen dominance, where estrogen's fluid-retaining effects go unchecked.
This is why perimenopausal bloating often feels like an amplified version of premenstrual bloating — because the underlying mechanism is similar, just more intense and less predictable.
How Hormones Slow Your Digestion
Progesterone has a direct relaxing effect on smooth muscle tissue — including the muscles of your digestive tract. When progesterone fluctuates, gut motility (the speed at which food moves through your system) becomes inconsistent.
This can lead to:
Slower gastric emptying (food sitting in your stomach longer)
Increased gas production as food ferments in the intestines
Alternating constipation and looser stools
A general feeling that your digestion just isn't working the way it used to
Estrogen also affects bile production and gut transit time. When both hormones are in flux, your entire digestive rhythm can feel disrupted.
The Cortisol and Gut Connection
Perimenopause doesn't happen in isolation. Many women in their 40s and early 50s are navigating significant stress — from career demands, aging parents, teenagers, relationship shifts, financial pressures, or simply the cumulative weight of doing too much for too long.
Chronic stress elevates cortisol, which:
Slows digestion (your body deprioritizes gut function during stress)
Increases visceral fat storage around the midsection
Disrupts the gut microbiome
Worsens inflammation, which can increase bloating
The hormonal shifts of perimenopause can also make your stress response more reactive. Many women describe feeling "wired" or unable to wind down — which keeps cortisol elevated and the gut in a perpetual state of low-grade disruption.
New Food Sensitivities During Perimenopause
Here's something that catches many women off guard: foods you've eaten your entire life without issues can suddenly start causing problems during perimenopause.
This happens because:
Declining estrogen affects the gut lining, potentially increasing intestinal permeability
Changes in the gut microbiome alter how certain foods are digested
Histamine tolerance can decrease during perimenopause, making fermented foods, aged cheeses, wine, and certain fruits more problematic
Inflammatory responses may be heightened
Common new triggers include:
Dairy (especially cow's milk)
Gluten or wheat products
Cruciferous vegetables (broccoli, cauliflower, Brussels sprouts)
Onions and garlic (high in FODMAPs)
Alcohol — particularly wine and beer
Artificial sweeteners
Caffeine in large amounts
This doesn't mean you need to eliminate everything. But noticing patterns between what you eat and when you bloat is one of the most empowering steps you can take.


What Women Actually Experience
Real Patterns Women Describe
In perimenopause communities, in our reader surveys, and across clinical literature, certain themes repeat with striking consistency:
"My digestion changed overnight." Women describe going from having a predictable, comfortable gut to dealing with daily bloating, gas, and irregularity — often with no change in diet.
"The bloating is cyclical, but my cycles aren't." Many women notice that bloating worsens at certain times of the month — but as periods become irregular, the pattern becomes harder to track.
"I've been tested for everything." Celiac disease. Ovarian cysts. IBS. SIBO. Many women undergo extensive testing, and while some do find co-occurring conditions, others hear "everything looks normal" — which feels both reassuring and invalidating.
"It's worst when I'm stressed and not sleeping." Almost universally, women report that bloating intensifies during periods of emotional stress, poor sleep, or both.
"I don't recognize my own body." The physical changes — bloating, shifting weight distribution, skin changes — can feel disorienting. This isn't vanity. It's a genuine loss of familiarity with your own body.
"I Look Six Months Pregnant by 3 PM"
This phrase — or some version of it — appears in nearly every perimenopause bloating discussion. And it deserves to be taken seriously rather than laughed off.
The visible distension that many women experience is not subtle. It can change clothing choices, affect confidence, and create genuine anxiety about social situations or professional settings.
This is a real, physical symptom with hormonal origins. It's not about discipline. It's not about what you had for lunch. And acknowledging its impact — emotionally as well as physically — is an important first step.
What Science Says About Hormones and Bloating
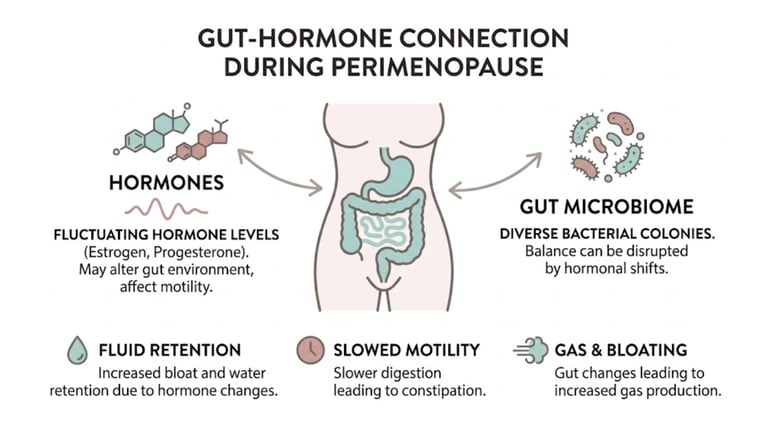
The Gut-Hormone Axis Explained Simply
Your gut and your reproductive hormones are in constant communication. This relationship — sometimes called the gut-hormone axis or estrobolome — works in both directions:
Hormones affect the gut: Estrogen and progesterone influence gut motility, fluid retention, microbiome composition, and intestinal permeability.
The gut affects hormones: Your gut bacteria play a role in metabolizing and recycling estrogen. When the microbiome is disrupted, estrogen metabolism can become less efficient — potentially worsening symptoms.
During perimenopause, this bidirectional system is destabilized. Hormone fluctuations disrupt the gut, and gut disruption can, in turn, amplify hormonal symptoms. It becomes a feedback loop.
Research published in journals like Maturitas and The Journal of Clinical Endocrinology & Metabolism has explored how the menopausal transition affects gastrointestinal function — though bloating specifically remains under-researched compared to hot flashes and mood changes.
What's Established, What's Probable, and What's Still Debated
Being transparent about what we know — and what we don't yet fully understand — is essential for building trust. The hormonal link to bloating is real and well-supported. The exact mechanisms and best treatments are still being refined.
When Is Perimenopause Bloating Worst?
Cycle Patterns and Hormonal Timing
If you're still having periods (even irregular ones), you may notice bloating tends to peak:
In the luteal phase (the week or two before your period), when progesterone rises and then drops
During estrogen surges — which can happen unpredictably in perimenopause, sometimes producing much higher estrogen levels than your body experienced in your 30s
Around ovulation — when estrogen peaks sharply
When you skip a period — the prolonged hormonal limbo of a missed cycle can create extended bloating episodes
For women whose periods have become very irregular or have stopped, the timing becomes less predictable — but the bloating often continues, driven by residual hormonal fluctuations and the other factors described above.
Lifestyle Triggers That Amplify Bloating
Hormones set the stage. But certain habits and circumstances can turn the volume up significantly:
Eating too fast — swallowing air and not chewing thoroughly increases gas production
Large meals — an already-slow digestive system struggles with volume
Dehydration — paradoxically, not drinking enough water causes your body to retain more fluid
High sodium intake — processed foods, restaurant meals, and snack foods promote water retention
Sedentary days — movement helps gas move through the intestines; sitting all day traps it
Alcohol — irritates the gut lining, disrupts the microbiome, and worsens water retention
Chronic stress without recovery — keeps cortisol high and digestion sluggish
Inadequate fiber (or sudden excess fiber) — both extremes cause problems
Is Perimenopause Bloating Dangerous?
When Bloating Is Hormonal and Harmless
In most cases, perimenopause-related bloating is uncomfortable but not medically dangerous. It tends to:
Fluctuate rather than progressively worsen
Respond (at least partially) to dietary and lifestyle changes
Coexist with other recognizable perimenopause symptoms
Not be accompanied by alarming clinical signs
It can, however, significantly affect quality of life — and that matters. Discomfort, self-consciousness, disrupted eating patterns, and anxiety about underlying causes are all valid concerns worth addressing.
Red Flags That Need Medical Attention
Please consult a healthcare provider if you experience:
Persistent bloating that doesn't fluctuate and lasts more than 2–3 weeks without relief
Bloating with unexplained weight loss (not related to intentional dieting)
Blood in your stool or significant changes in bowel habits
Severe abdominal pain — not just discomfort, but sharp or escalating pain
Loss of appetite or feeling full after eating very little (early satiety)
Pelvic pressure or pain, especially with urinary frequency
Family history of ovarian or colon cancer
These symptoms may indicate conditions such as ovarian pathology, inflammatory bowel disease, or other gastrointestinal conditions that require evaluation. Persistent, unexplained bloating in women over 40 should always be discussed with a doctor — not to create fear, but to rule out anything that needs attention.
How Long Does Perimenopause Bloating Last?
Every woman's timeline is different, but here's what the general pattern looks like:
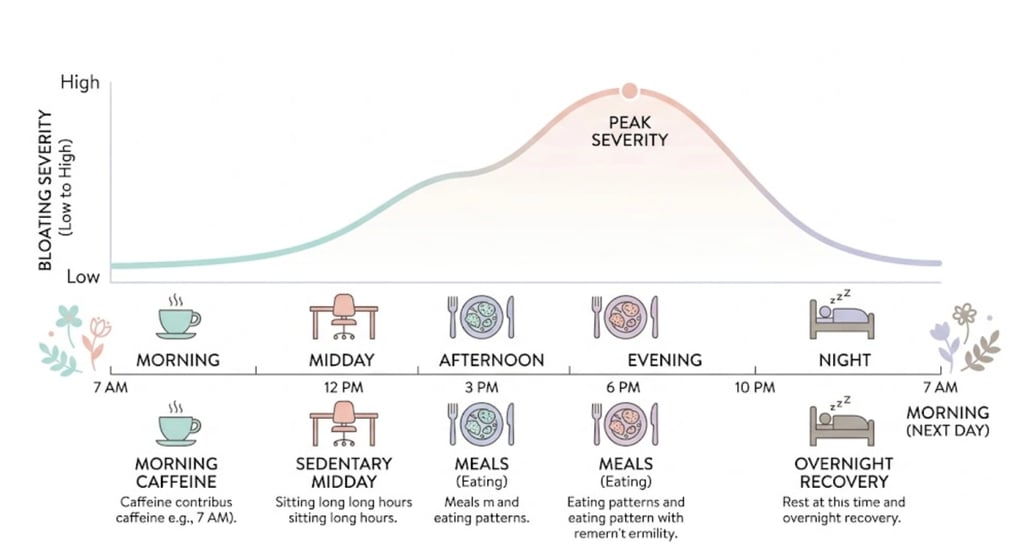
Individual bloating episodes often follow a daily rhythm — minimal in the morning, peaking in the afternoon or evening — and resolve overnight.
Cyclical bloating (tied to hormonal fluctuations) typically lasts a few days to two weeks per cycle in early perimenopause, but becomes less predictable as cycles become irregular.
The symptom overall tends to be most intense during mid-to-late perimenopause, when hormonal fluctuations are at their most dramatic.
Many women experience improvement as they transition into postmenopause and hormone levels stabilize — though some continue to deal with milder bloating related to age-related digestive changes.
Dietary and lifestyle interventions (detailed below) can reduce bloating significantly within weeks — even while hormones are still in flux.
The reassuring truth: for most women, the worst of it is a phase, not a permanent state.
12 Gentle Ways to Reduce Perimenopause Bloating
These strategies are drawn from gastroenterological guidance, hormonal health research, and the real-world experience of thousands of perimenopausal women. Start with the ones that feel most relevant to you.
Eating Patterns That Calm the Gut
1. Eat smaller, more frequent meals.
A sluggish digestive system handles smaller volumes more efficiently. Three moderate meals plus one or two small snacks often works better than two or three large meals.
2. Slow down and chew thoroughly.
This sounds basic — but it's transformative. Chewing well reduces the amount of air you swallow and gives your digestive enzymes more time to work. Put your fork down between bites. Aim for 20 minutes per meal minimum.
3. Stop eating 2–3 hours before bed.
Lying down with a full stomach worsens bloating and can disrupt sleep. Give your digestive system a clear window to process before you go horizontal.
Foods to Prioritize — and Foods to Ease Back On
4. Prioritize anti-bloating foods.
Some foods actively support digestion and reduce gas:
Ginger (fresh or as tea — a natural prokinetic that speeds gastric emptying)
Fennel and fennel tea (relaxes smooth muscle in the GI tract)
Cucumber and celery (natural diuretics that reduce water retention)
Cooked vegetables over raw (easier to digest during hormonal flux)
Peppermint tea (helps relax the intestinal walls)
5. Identify your personal triggers.
Keep a simple food-symptom journal for 2–3 weeks. Note what you eat and when bloating occurs. Common perimenopausal triggers include dairy, wheat, cruciferous vegetables, onions, garlic, artificial sweeteners, and alcohol. You don't need to eliminate everything — just notice your patterns.
6. Support your gut microbiome.
Consider incorporating:
Probiotic-rich foods (yogurt, kefir, sauerkraut — if tolerated)
Prebiotic fibers (oats, flaxseeds, bananas — introduce slowly)
A high-quality probiotic supplement with strains supported by research (such as Lactobacillus and Bifidobacterium species)
Movement, Posture, and Digestive Support
7. Walk after meals.
Even 10–15 minutes of gentle walking after eating significantly improves gut motility and reduces post-meal bloating. This is one of the most evidence-supported strategies available — and one of the simplest.
8. Practice abdominal massage.
Lying on your back, use gentle clockwise circular motions around your abdomen (following the path of the colon). This can help move trapped gas and stimulate peristalsis. Do it for 5 minutes before bed or when bloating is at its peak.
9. Check your posture.
Sitting hunched at a desk compresses your abdominal organs and slows digestion. Sit tall, with your feet flat on the floor. Consider a standing desk for part of your workday.
Stress, Sleep, and the Nervous System
10. Activate your "rest and digest" mode.
Your parasympathetic nervous system governs digestion. To activate it:
Take 5 slow, deep breaths before eating (this alone can improve digestion)
Eat without screens or multitasking when possible
Practice 10 minutes of daily meditation, breathwork, or gentle yoga
Consider vagus nerve stimulation techniques (humming, gargling, cold water on the face)
11. Protect your sleep.
Poor sleep increases cortisol, disrupts the microbiome, and worsens every digestive symptom — including bloating. Prioritize 7–8 hours. Keep the room cool. Consider magnesium glycinate before bed, which supports both sleep quality and smooth muscle relaxation in the gut.
When to Explore Medical or Hormonal Support
12. Talk to your healthcare provider.
If bloating is persistent and significantly affecting your quality of life, medical options may include:
Hormone therapy (HT) — stabilizing estrogen and progesterone can reduce fluid retention and improve gut motility in some women
Low-FODMAP diet guidance — ideally with a registered dietitian, to systematically identify trigger foods
Testing for co-occurring conditions — such as SIBO (small intestinal bacterial overgrowth), thyroid dysfunction, or food intolerances
Medication review — some common medications (metformin, certain supplements, antidepressants) can worsen bloating
Advocating for yourself doesn't mean something is seriously wrong. It means you deserve to feel comfortable in your own body.
Frequently Asked Questions
Is bloating a symptom of perimenopause?
Yes. Bloating is one of the most commonly reported perimenopause symptoms. Fluctuating estrogen and progesterone affect water retention, gut motility, and the microbiome — all of which contribute to abdominal distension and discomfort.
Why is my stomach so bloated during perimenopause?
Estrogen surges cause your body to retain fluid, while progesterone fluctuations slow digestion and increase gas. Stress-related cortisol and changes to your gut bacteria can amplify the effect.
Does perimenopause bloating go away?
For most women, hormonal bloating improves as the transition into postmenopause progresses and hormone levels stabilize. Dietary and lifestyle changes can significantly reduce symptoms even during the transition itself.
What helps with perimenopause bloating?
Smaller meals, slower eating, regular walking, hydration, stress management, and identifying personal food triggers are the most effective starting strategies. Some women also benefit from hormone therapy or professional dietary guidance.
Can perimenopause cause bloating and gas?
Yes. Progesterone relaxes the smooth muscles of the digestive tract, slowing transit time and increasing gas production. This is the same mechanism that causes bloating during the premenstrual phase — but amplified by the hormonal chaos of perimenopause.
Should I be worried about perimenopause bloating?
Occasional, fluctuating bloating during perimenopause is usually hormonal and harmless. However, persistent bloating that doesn't fluctuate, combined with pelvic pain, unexplained weight loss, or changes in bowel habits, should be evaluated by a healthcare provider.
Your Belly Is Not the Problem — Your Hormones Are Shifting
If you've been sucking in your stomach, canceling dinner plans, or lying awake wondering what's wrong with you — please stop blaming yourself.
Perimenopause bloating is a physiological response to a major hormonal transition. It's not a character flaw. It's not because you ate bread. And it's not something you should have to suffer through in silence.
Your body is doing something big right now. It's recalibrating systems that have been running on a particular hormonal pattern for decades. That recalibration isn't always comfortable — but it is temporary, it is manageable, and it is something you can navigate with the right information and support.
Start where you can. Be patient with the process. And know that you are not the only woman standing in front of her mirror at 4 PM wondering where her waistline went.
You're in very good company.
Ready to take the next step?
(https://perimenopausecompass.com/free-14-day-tracker) to find your personal triggers.
Get the Perimenopause Nutrition Protocol to support your nervous system from the inside out.
Visit our (https://perimenopausecompass.com/start-here) page for more foundational guidance.
Get the Perimenopause Nutrition Protocol ($29 + bonus) → https://perimenopausecompass.gumroad.com/l/iecoc
______________________________________
Disclaimer Education only — not medical advice. Consult a qualified healthcare professional for diagnosis and treatment.
Sources / References
Perimenopause Compass
Contact
hello@perimenopausecompass.com
© 2026 All rights reserved.
