Early Signs of Perimenopause Most Women Ignore
Many early signs of perimenopause feel like stress or aging. Discover the subtle symptoms most women miss — and why recognizing them early matters.
Perimenopause Compasss
2/11/202614 min read


Something feels off. Not dramatically wrong — just… different.
Maybe your sleep has changed. Maybe your periods are slightly shorter. Maybe you've been more anxious lately, or your brain feels foggy in ways it didn't before. Maybe you Googled "why am I so tired at 42" or "sudden anxiety for no reason" before landing here.
If any of this sounds familiar — you may be experiencing the early signs of perimenopause. And you're far from alone in not recognizing them.
Most women know about hot flashes and missed periods. But perimenopause often starts with symptoms that are quieter, subtler, and easier to dismiss — as stress, burnout, aging, or simply "nothing."
This article covers the early signs most women overlook, explains why they happen, and helps you figure out whether what you're feeling might be the beginning of your hormonal transition.
What Is Perimenopause — And When Does It Actually Start?
Before we get to the signs, let's get clear on what perimenopause actually is — because there's still a lot of confusion.
The Difference Between Perimenopause and Menopause
Menopause is a single point in time: the day that marks 12 consecutive months without a period. The average age is 51.
Perimenopause is the transition leading up to that point. It's the years during which your hormones — primarily estrogen and progesterone — begin to fluctuate and gradually decline.
Think of menopause as the destination. Perimenopause is the entire road trip getting there — and it can be a bumpy one.
Why It Can Start Earlier Than You Think
Most women expect menopause-related changes in their late 40s or early 50s. But perimenopause can begin much earlier.
According to the Cleveland Clinic, perimenopause typically starts in a woman's mid-40s, but it can begin as early as the mid-to-late 30s. The transition lasts an average of 4 to 8 years, though some women experience it for longer.
This means a woman who reaches menopause at 51 may have entered perimenopause at 43 or even earlier — years before she'd ever suspect it.
And that's precisely why so many early signs get missed.
Why Are Early Signs So Easy to Miss?
The "Too Young" Myth
One of the biggest barriers to recognizing early perimenopause is the belief that you're "too young."
If you're 40 or 42 or even 38 and you mention symptoms to a friend — or even a doctor — you might hear: "You're too young for that."
But biology doesn't follow a calendar. Hormonal shifts are gradual, not sudden. They don't announce themselves with a clear starting point. And they begin well before periods become visibly irregular.
The "too young" narrative means millions of women spend months or years attributing legitimate hormonal symptoms to other causes.
When Symptoms Look Like Stress, Aging, or Burnout
Early perimenopause symptoms have a frustrating characteristic: they mimic other things.
New anxiety? Must be work stress.
Fatigue? Probably just a busy schedule.
Brain fog? Maybe not enough sleep.
Irritability? Life is overwhelming right now.
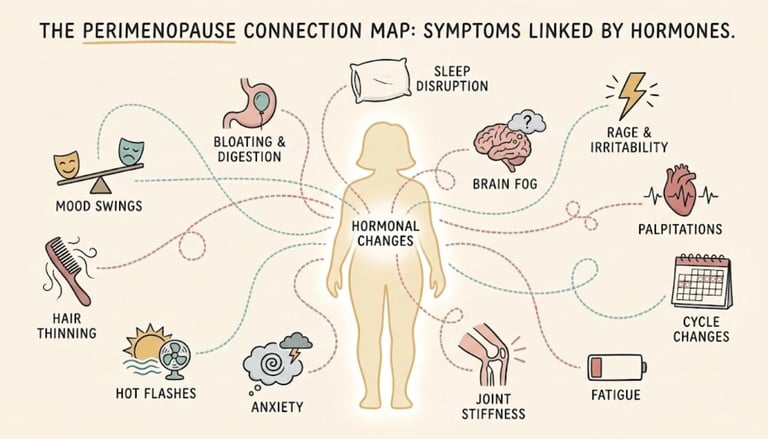
Each symptom, in isolation, seems explainable. It's only when you look at the pattern — multiple subtle changes appearing around the same time — that the picture becomes clearer.
This is what makes early perimenopause so easy to overlook. No single sign screams "hormones." But together, they whisper it.
12 Early Signs of Perimenopause Most Women Don't Recognize
These aren't the classic symptoms you'll find on the first page of every menopause website. These are the early, subtle, frequently dismissed signs that often appear years before hot flashes or missed periods.
1. Your Period Is Slightly Different — But Still "Regular"
You might still be getting your period every month. But something small has shifted:
It's heavier than it used to be — maybe just for one or two days
Or it's lighter and shorter
The timing has shifted by a few days
You're getting more clotting than before
Your PMS window feels longer or more intense
These changes can be so gradual that you barely notice. But subtle shifts in your period are often the very first hormonal signal that your ovarian function is changing.
2. Sleep Just Doesn't Feel the Same Anymore
You might not have full-blown insomnia. But sleep quality has changed:
You wake up at 3 or 4 a.m. and can't fall back asleep
You sleep a full night but wake up feeling unrested
You feel wired at bedtime even though you're exhausted
Your sleep feels lighter — you wake at the slightest noise
Declining progesterone — which often drops before estrogen becomes noticeably irregular — has a direct effect on sleep quality. Progesterone enhances GABA, your brain's calming neurotransmitter. Less progesterone can mean less deep, restorative sleep.
3. Anxiety That Appeared Out of Nowhere
This is one of the most commonly overlooked early signs.
Women who have never been anxious suddenly experience:
A low-level sense of dread or unease
Ruminating thoughts, especially at night
Physical anxiety — tight chest, racing heart, tension — without a clear trigger
A feeling of being emotionally fragile in a way that's unfamiliar
Estrogen modulates serotonin and GABA — two neurotransmitters central to mood stability and calm. When estrogen begins to fluctuate, your brain's chemistry shifts — sometimes before any physical symptoms appear.
If your anxiety feels new, unexplained, and out of character, perimenopause belongs on the list of possible explanations.
4. Shorter Menstrual Cycles
This one hides in plain sight.
Your cycle might go from a reliable 28–30 days to 25 or 26 days. You might notice that your periods seem to come "early" more often.
Shortened cycles are a classic early sign of perimenopause. They typically result from shorter follicular phases — meaning your body is moving through the first half of the cycle faster as follicle reserves decline.
It's subtle. You might not even notice unless you're tracking. But it's one of the most reliable early indicators.
5. Fatigue That Rest Doesn't Fix
Not the tiredness you feel after a bad night. Something deeper.
A bone-deep exhaustion that doesn't improve with more sleep
Feeling like your battery doesn't fully recharge anymore
Needing significantly more rest to function at your normal level
Energy crashes in the afternoon, even when you've eaten well
This kind of fatigue is multifactorial in perimenopause: it's connected to disrupted sleep, fluctuating cortisol, hormonal instability, and sometimes subtle changes in thyroid function that occur alongside the hormonal transition.
6. Brain Fog and Word-Finding Problems
You walk into a room and forget why. You search for a word that was on the tip of your tongue. You read a paragraph and realize you absorbed nothing.
Perimenopausal brain fog is real and well-documented. Research from the Study of Women's Health Across the Nation (SWAN) confirms that cognitive changes — particularly in memory and processing speed — are associated with the menopausal transition.
It's not dementia. It's not permanent decline. It's your brain adapting to a shifting hormonal environment — and estrogen plays a significant role in verbal memory, attention, and executive function.
But because no one tells women this might happen in their early 40s, many spend months worrying that something is seriously wrong.
7. Rage, Irritability, or Emotional Overwhelm
There's a specific kind of anger that women in early perimenopause describe — and it's different from everyday frustration:
A disproportionate rage over minor things
Feeling like you have zero patience — with your kids, your partner, your colleagues
An emotional rawness, as though your skin is thinner
Crying more easily, or swinging between anger and tears
This isn't a character flaw. It's a neurochemical shift. Fluctuating estrogen affects serotonin and dopamine pathways, which directly influence emotional regulation.
Many women say this symptom was the most confusing — because it felt like they had changed, when really, their hormones had.
8. New or Worsening PMS
If your PMS has become noticeably worse — or if you're suddenly experiencing PMS when you never really did before — pay attention.
Signs include:
Breast tenderness that feels more intense
Bloating that lasts longer
Mood swings in the luteal phase that feel amplified
Headaches or migraines around your period that are new or worse
In early perimenopause, progesterone drops faster than estrogen, creating a relative estrogen dominance in the second half of your cycle. This hormonal imbalance is often what makes PMS suddenly feel unbearable.
9. Changes in Libido You Can't Explain
Desire is complex — it's not purely hormonal. But when your libido shifts noticeably and you can't attribute it to relationship dynamics, stress, or medication, hormones may be playing a role.
Early perimenopausal changes in libido can include:
A general decrease in spontaneous desire
Feeling physically less responsive than before
Changes in vaginal lubrication (subtle at first)
A shift in what arouses you — or a sense that desire feels more "effortful"
Testosterone — yes, women produce it too — begins declining from the late 30s onward, and fluctuating estrogen can affect genital blood flow and nerve sensitivity.
10. Joint Stiffness and Random Aches
You wake up with stiff fingers. Your hips ache for no reason. Your shoulders feel tight even though you haven't done anything strenuous.
Estrogen has anti-inflammatory properties and helps maintain joint lubrication. As levels fluctuate, many women notice:
Morning stiffness that takes a while to ease
Aching joints — hips, knees, hands, shoulders
A general sense of physical stiffness that wasn't there before
This symptom is so frequently overlooked that many women see a rheumatologist before anyone considers hormones.
11. Heart Palpitations That Come and Go
A sudden flutter. A skipped beat. A moment where your heart feels like it's pounding for no reason.
Perimenopausal heart palpitations are surprisingly common and usually benign. They're linked to estrogen's role in regulating heart rhythm and the autonomic nervous system.
They tend to appear:
At night or when lying down
Around ovulation or just before a period
During periods of higher stress
That said, new heart palpitations should always be evaluated by a doctor to rule out cardiac causes — even if perimenopause is the most likely explanation.
12. A Gut Feeling That Something Has Shifted
This isn't a clinical symptom. You won't find it in a textbook. But it's something women describe over and over:
"I just feel different. Something in my body has changed, but I can't point to exactly what."
It might manifest as:
Feeling less resilient — physically, emotionally, or both
A sense that your body doesn't recover the way it used to
Subtle changes in your skin, hair texture, or body composition
A quiet awareness that a new chapter has begun
Trust that feeling. Your body often knows before your lab results do.
What Women Actually Experience — In Their Own Words
"I Thought I Was Burning Out"
"At 43, I was convinced I had burnout. I was exhausted, foggy, emotional. I took time off work, slept more, meditated — and nothing changed. It wasn't until a friend mentioned perimenopause that I even considered it. My doctor confirmed my progesterone had dropped significantly. I wasn't burned out. My hormones had shifted."
"My Doctor Said It Was Just Stress"
"I went to my GP three times over a year. Anxiety, insomnia, heart palpitations. Every time: 'It's probably stress. Try relaxation techniques.' It took me finding a menopause-informed doctor to finally get someone to connect the dots. I wish I'd known earlier that these were hormonal symptoms — I spent a year thinking I was falling apart."
"I Didn't Connect the Dots for Years"
"Looking back, my perimenopause started at 41. Shorter cycles. Worse PMS. Waking at 4 a.m. Occasional rage that wasn't like me. But each symptom seemed separate. It was only when I read an article listing the early signs together that I thought — oh. That's ALL of these. It was a relief to finally have a name for it."
These stories aren't unusual. They're the norm. And they highlight why education about early perimenopause signs matters so much — because recognition is the first step toward getting the right support.
What Science Says About Early Perimenopause
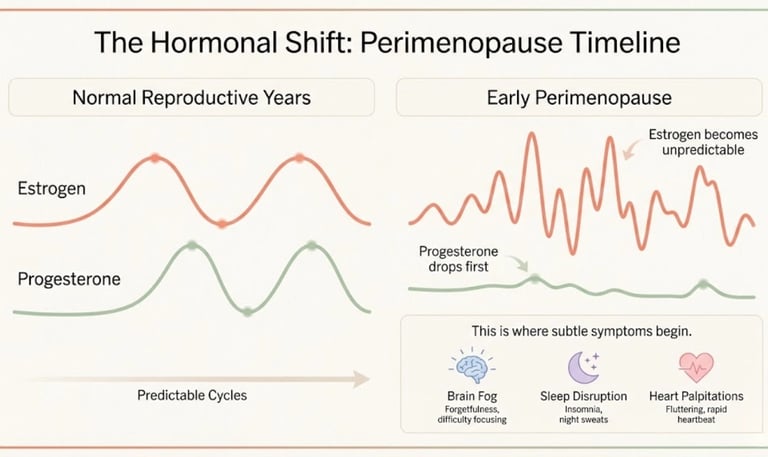
The Hormonal Shifts Behind the Subtle Symptoms
Perimenopause isn't a simple "estrogen drops" story. What actually happens is more nuanced:
Progesterone declines first. As ovulation becomes less consistent, progesterone — which is only produced after ovulation — drops. This is often why sleep, mood, and PMS symptoms appear before any period changes.
Estrogen becomes erratic. Rather than steadily declining, estrogen swings — sometimes spiking to levels higher than in your 20s, then crashing. These wild fluctuations cause many of the acute symptoms: anxiety, hot flashes, mood swings.
FSH (Follicle-Stimulating Hormone) rises. Your brain's pituitary gland produces more FSH to try to stimulate ovaries that are becoming less responsive. This is the hormonal signal doctors sometimes test for — though it's unreliable in early perimenopause.
Testosterone gradually declines. This slow reduction — beginning well before menopause — contributes to changes in energy, libido, and muscle mass.
The key insight: early perimenopause is characterized by hormonal instability, not deficiency. Your levels aren't just low — they're unpredictable. And that unpredictability is what makes symptoms come and go, shift and evolve.
Why Standard Blood Tests Often Miss It
If you've had blood work done and been told your hormones are "normal," that doesn't necessarily rule out perimenopause.
Here's why:
Estrogen and progesterone fluctuate daily in perimenopause. A single blood draw captures one moment — not the pattern.
FSH levels are highly variable during the transition and can appear "normal" one day and elevated the next.
Standard reference ranges were designed for premenopausal or postmenopausal women — not for women in the volatile middle ground.
The Stages of Reproductive Aging Workshop (STRAW+10) criteria — the gold standard for classifying reproductive aging — emphasizes that early perimenopause is a clinical diagnosis, based primarily on symptoms and menstrual cycle changes, not blood tests alone.
If you suspect early perimenopause, the most important thing is finding a provider who understands this and won't dismiss your symptoms because a single lab panel looks "fine."
What Research Confirms vs. What's Still Being Studied
Scientifically established:
Perimenopause can begin 4–8+ years before menopause
Hormonal fluctuations during the transition directly affect sleep, mood, cognition, and vasomotor function
Progesterone typically declines before estrogen becomes noticeably irregular
Cognitive changes during perimenopause are real and typically temporary
Probable (supported by growing evidence):
Anxiety and mood symptoms may precede vasomotor symptoms as the earliest sign for some women
Gut microbiome changes during perimenopause may influence symptom severity
Inflammation increases during the transition, contributing to joint pain and fatigue
Still debated or under-researched:
Whether early perimenopause onset predicts greater symptom severity
The role of epigenetics and lifestyle in timing of the transition
Optimal diagnostic criteria for early-stage perimenopause
Whether early intervention improves long-term outcomes
This article is for educational purposes and does not replace medical advice. If you're experiencing symptoms that concern you, consult a healthcare provider — ideally one with training in menopause medicine.
How to Know If It's Perimenopause — Or Something Else
Several of the symptoms described above overlap with other conditions. Ruling them out — or recognizing them alongside perimenopause — is important.
Perimenopause vs. Thyroid Issues
Hypothyroidism (underactive thyroid) can cause fatigue, brain fog, weight changes, mood shifts, and cycle irregularities — all of which overlap with perimenopause.
Key differences:
Perimenopause vs. Depression or Anxiety Disorder
New-onset mood symptoms in a woman over 40 can look identical to clinical depression or generalized anxiety. And sometimes, it is both — perimenopause can trigger or worsen pre-existing mental health conditions.
Clues that hormones are playing a role:
Symptoms are cyclical — worse at certain points in your menstrual cycle
They appeared without a clear psychological trigger
You've never experienced them before, or they feel qualitatively different from past episodes
They're accompanied by other perimenopausal signs (cycle changes, sleep disruption, physical symptoms)
This doesn't mean you shouldn't seek mental health support — you absolutely should if you're struggling. But it does mean that a hormonal lens should be part of the conversation.
When to See Your Doctor — And What to Ask
Schedule an appointment if:
You're experiencing multiple symptoms from the list above
Symptoms are affecting your quality of life, relationships, or ability to function
You want to rule out other causes (thyroid, anemia, etc.)
You're interested in exploring treatment options
What to bring to your appointment:
A symptom log — at least 2–4 weeks of notes on what you're experiencing
Your menstrual cycle history — any changes in length, flow, or regularity
A list of specific questions, such as:
"Could my symptoms be related to perimenopause?"
"Should we check my thyroid function?"
"What are my options if this is hormonal?"
"Would you consider a referral to a menopause specialist?"
Important: Not all doctors are well-trained in perimenopause. A recent survey published in Menopause journal found that many physicians receive little formal education on menopause management. If you feel dismissed, seeking a NAMS-certified menopause practitioner (searchable at menopause.org) can make a significant difference.
What You Can Do Right Now
You don't have to wait for a diagnosis to start supporting your body through this transition.
Start Tracking Your Symptoms Today
Awareness is the most powerful first step. When you track your symptoms alongside your cycle, patterns emerge that are invisible otherwise.
What to log daily (it takes 2 minutes):
Energy level (1–5)
Sleep quality (1–5)
Mood (key emotions)
Any physical symptoms (joint pain, headache, palpitations)
Cycle day (if still menstruating)
Notable stressors or events
After 4–6 weeks, review your log. You may see clear connections between your cycle phase and your symptoms — which is both validating and clinically useful.
Lifestyle Shifts That Support Hormonal Balance
These aren't miracle cures. But they're evidence-supported strategies that can reduce symptom severity and support your body during hormonal instability:
Prioritize protein at every meal — supports stable blood sugar, which helps reduce cortisol spikes and energy crashes
Strength training 2–3x per week — maintains muscle mass, supports bone density, improves insulin sensitivity, and can boost mood
Reduce alcohol — even moderate alcohol can worsen sleep disruption, hot flashes, anxiety, and hormonal imbalance during perimenopause
Optimize sleep environment — cool room, consistent schedule, limited screens before bed
Manage stress intentionally — your stress response system is more reactive now. Breathwork, walking, nature, and boundaries aren't luxuries — they're physiological necessities
Consider anti-inflammatory nutrition — omega-3 fatty acids, colorful vegetables, and reducing ultra-processed foods may help manage inflammation-related symptoms
When to Consider Medical Support
Lifestyle strategies are foundational — but they're not always enough. If your symptoms are moderate to severe or significantly impacting your life, medical options exist and are worth discussing:
Hormone therapy (HT) — effective for vasomotor symptoms, sleep, mood, and bone protection. Current evidence supports its use in appropriate candidates.
Micronized progesterone — may improve sleep and mood specifically.
Low-dose SSRIs/SNRIs — effective for mood symptoms and hot flashes, even in non-depressed women.
CBT-I (Cognitive Behavioral Therapy for Insomnia) — the gold standard non-drug treatment for insomnia.
You don't have to "push through" perimenopause unaided. Getting support is not weakness — it's wisdom.
You're Not Imagining It — And You're Not Too Young
If you've spent months — or years — feeling like something was off but couldn't name it, we hope this article helps.
The early signs of perimenopause are easy to miss because:
They start gradually
They mimic other things
No one tells us to expect them this early
Many healthcare providers don't recognize them either
But knowing changes everything. When you understand that your anxiety, your fatigue, your foggy brain, and your changing cycle might be connected — and that there's a hormonal explanation — something shifts.
You stop blaming yourself. You stop wondering if you're imagining it. You start making informed choices about your health.
Perimenopause isn't a disease. It's a natural biological transition. But natural doesn't mean you have to suffer through it silently or uninformed.
You deserve to understand what your body is doing. And you deserve support while it does it.
FAQ — Early Signs of Perimenopause
Q: What is usually the first sign of perimenopause?
A: For many women, the first sign is a subtle change in menstrual cycle length — often shorter cycles — or a shift in sleep quality. New or unexplained anxiety is also a common early indicator that often goes unrecognized.
Q: Can perimenopause start at 40?
A: Yes. Perimenopause typically begins in the mid-40s but can start in the late 30s or early 40s. This is considered normal, not early menopause. It simply means your hormonal transition has begun.
Q: How do I know if it's perimenopause or something else?
A: Look for multiple subtle symptoms appearing together — sleep changes, mood shifts, cycle irregularities, fatigue. A healthcare provider can help rule out thyroid issues, anemia, or other conditions with similar symptoms.
Q: Can you be perimenopausal with regular periods?
A: Absolutely. Many women continue having regular periods in early perimenopause. Hormonal fluctuations — especially in progesterone — can cause symptoms well before your cycle becomes visibly irregular.
Q: Do blood tests confirm perimenopause?
A: Not reliably in early stages. Hormone levels fluctuate significantly during perimenopause, so a single blood test can appear normal. Diagnosis is primarily based on symptoms, age, and menstrual cycle changes.
Q: Should I see a doctor for early perimenopause signs?
A: Yes, especially if symptoms affect your quality of life. A menopause-informed doctor can rule out other causes, validate your experience, and discuss management options including lifestyle changes and hormone therapy.
Ready to take the next step?
https://perimenopausecompass.com/free-14-day-tracker to build your foundation.
Get the Perimenopause Nutrition Protocol to support your protein and mineral needs.
Visit our https://perimenopausecompass.com/start-here page for more resources.
Get the Perimenopause Nutrition Protocol ($29 + bonus) → https://perimenopausecompass.gumroad.com/l/iecoc
_________________________________________________
Disclaimer Education only — not medical advice. Consult a qualified healthcare professional for diagnosis and treatment.
Sources / References
Get the Perimenopause Nutrition Protocol ($29 + bonus)
Get the Perimenopause Nutrition Protocol ($29 + bonus)
A thyroid panel (TSH, Free T4, Free T3, antibodies) can help differentiate. And note: both conditions can coexist, since thyroid dysfunction becomes more common as women age.
Perimenopause Compass
Contact
hello@perimenopausecompass.com
© 2026 All rights reserved.
