Perimenopause Dizziness: Why It Happens & What Helps
Feeling dizzy during perimenopause? You're not imagining it. Learn why hormonal shifts cause dizziness, what triggers to watch for, and gentle ways to find relief. Perimenopause Dizziness
EDUCATIONAL
3/21/20269 min read
You're standing in the kitchen, making coffee, and the room tilts. Just slightly. Just enough to make you grab the counter. It passes in a few seconds, but the unease stays longer.
Or maybe it's not a tilt. Maybe it's a foggy, floating feeling — like you're slightly disconnected from the ground beneath you. It happens in meetings. In the grocery store. While you're driving.
You've probably Googled it more than once. You've probably also wondered: Is this normal? Is this perimenopause? Or is something else going on?
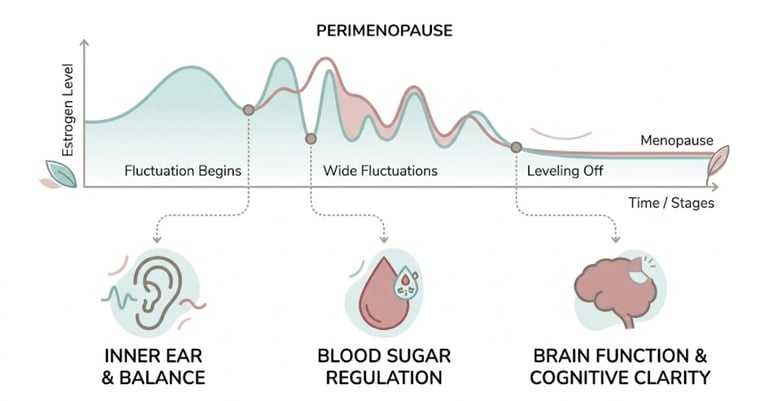
Here's the short answer: dizziness is a recognized but often overlooked symptom of perimenopause. Hormonal shifts — particularly fluctuating estrogen — can affect your inner ear, blood pressure regulation, blood sugar stability, and nervous system in ways that make dizziness more likely.
You're not imagining it. And you're far from alone.
This article walks you through the causes, the science, and — most importantly — what you can actually do about it.
This article is based on current medical knowledge and real-life experiences, but does not replace medical advice. If your dizziness is severe, sudden, or accompanied by other neurological symptoms, please consult a healthcare provider.
What Does Perimenopause Dizziness Actually Feel Like?
One of the most frustrating things about this symptom is how hard it is to pin down. Unlike a hot flash — which most people have at least heard of — dizziness during perimenopause can feel vague, intermittent, and difficult to describe to a doctor.
The Different Types of Dizziness Women Describe
Not all dizziness feels the same. Women in perimenopause typically report one or more of these sensations:
Lightheadedness — a feeling of almost fainting, often when standing up quickly
Unsteadiness — feeling "off-balance" while walking, as if the floor is slightly uneven
Floating sensation — a detached, dreamlike quality, as if you're not quite grounded
Spinning (vertigo) — the room or your surroundings seem to rotate, even briefly
Wooziness with hot flashes — dizziness that arrives alongside or just before a flush of heat
Post-meal dizziness — a wobbly feeling 1–2 hours after eating, often tied to blood sugar shifts
Some women experience one type consistently. Others cycle through several. And many say the unpredictability is what makes it so anxiety-inducing.
When Dizziness Shows Up (and Why It Catches You Off Guard)
Perimenopause dizziness tends to appear:
In the early-to-mid stages of perimenopause (often between 42 and 50)
Around the time of a period — or when a period was expected but didn't arrive
During or after a hot flash or night sweat
During high-stress periods or after poor sleep
When blood sugar drops (mid-morning, late afternoon, or after skipping meals)
What makes it especially confusing is that it rarely happens every day. It can disappear for weeks, then return with no obvious trigger. This inconsistency often leads women to doubt themselves — or to be dismissed by healthcare providers.


Why Does Perimenopause Cause Dizziness?
The short answer: hormones affect far more systems than most people realize.
Estrogen, in particular, has receptors in your inner ear, your blood vessels, your brain, and your autonomic nervous system. When estrogen levels become erratic — which is the hallmark of perimenopause — all of these systems can be temporarily destabilized.
The Estrogen–Inner Ear Connection
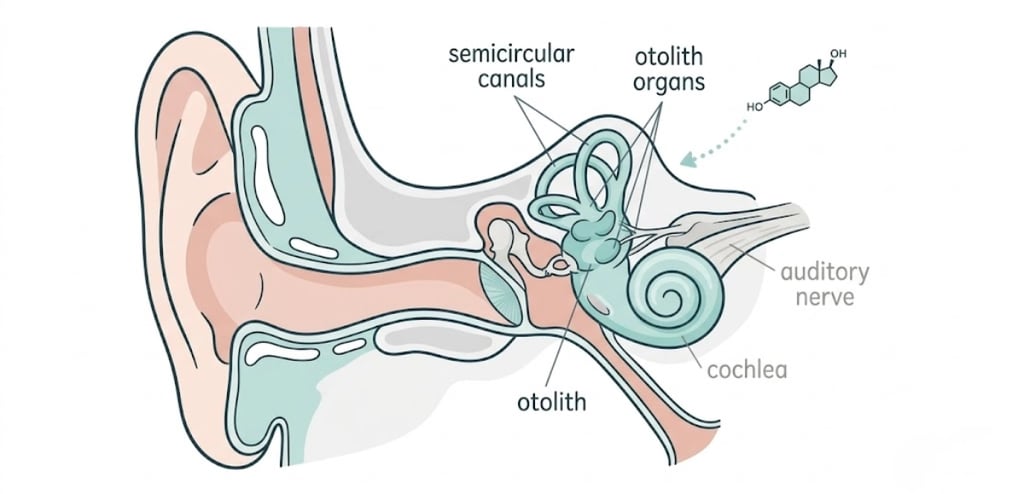
Your vestibular system (the balance center inside your inner ear) contains estrogen receptors. When estrogen levels drop or fluctuate sharply, fluid regulation in the inner ear can be disrupted. This can create sensations of dizziness, imbalance, or even brief episodes of vertigo.
Research published in Menopause: The Journal of The North American Menopause Society has explored how hormonal fluctuations may impact vestibular function — though this remains an active area of study.
Blood Sugar Swings and Hormonal Shifts
Estrogen and progesterone both play a role in how your body manages insulin and glucose. During perimenopause, these hormones fluctuate unpredictably, which can lead to:
Reactive hypoglycemia (blood sugar crashing after meals)
Increased insulin resistance
Shakiness, lightheadedness, or brain fog between meals
If you notice dizziness tends to happen when you haven't eaten for a while — or shortly after a carb-heavy meal — blood sugar instability may be a contributing factor.
The Role of Anxiety, Sleep, and Stress
Perimenopause doesn't happen in a vacuum. Many women in this stage are also navigating:
Increased anxiety or new-onset panic symptoms (often hormonally driven)
Disrupted sleep from night sweats, insomnia, or restless legs
Chronic stress from caregiving, career demands, or life transitions
All of these can independently cause dizziness. And when they combine with hormonal fluctuations, the effect can be amplified.
Anxiety-related dizziness, in particular, is extremely common in perimenopause and is often misidentified as a cardiac or neurological issue before the hormonal connection is made.
What Women Actually Experience
Real Patterns Women Report
In online perimenopause communities, in clinical surveys, and in our own reader feedback, certain patterns emerge again and again:
"It started around 44 and nobody told me it could be hormonal." Many women spend months — sometimes years — seeing ENTs, cardiologists, or neurologists before the hormonal link is considered.
"It's worse in the week before my period — or when I skip one." The premenstrual estrogen drop (or the extended low-estrogen phase of a missed cycle) is a common trigger.
"It comes with brain fog and fatigue." Dizziness rarely travels alone. Most women describe it as part of a cluster that includes cognitive fuzziness, tiredness, and sometimes heart palpitations.
"It's worse when I'm dehydrated or haven't slept." Lifestyle factors don't cause the dizziness on their own — but they lower the threshold at which hormonal fluctuations produce symptoms.
"I Thought Something Was Seriously Wrong"
This deserves its own space, because almost every woman who experiences perimenopause dizziness goes through a period of genuine fear.
When the room spins unexpectedly, when you feel faint at your desk, when you can't quite trust your own balance — it's natural to worry. The fear is valid. And it's compounded by the fact that most medical resources don't list dizziness among the "classic" symptoms of perimenopause.
If you've been checked for cardiac, neurological, and inner ear conditions and everything came back normal — hormonal fluctuation is a very reasonable explanation. It doesn't mean nothing is happening. It means something real is happening, and it has a name.
What Science Says About Hormones and Dizziness
Research on Estrogen and the Vestibular System
The relationship between hormones and balance is backed by a growing body of research, though it remains less studied than hot flashes or mood changes.
Here's what the evidence shows:
Estrogen receptors have been identified in the vestibular system (inner ear structures responsible for balance). This was documented in studies examining hormonal influences on labyrinthine function.
Women report more balance disturbances during hormonal transitions — including menstruation, pregnancy, and menopause — than during hormonally stable phases.
Hormone therapy (HT) has been associated with improvement in dizziness symptoms in some perimenopausal and menopausal women, suggesting a direct hormonal mechanism.
Migrainous vertigo (vestibular migraine) — a condition with strong hormonal triggers — becomes more common during the perimenopausal transition.
What's Established, What's Probable, and What's Still Debated
Transparency matters here. The hormonal link to dizziness is real and supported by evidence — but the research is still catching up to what millions of women already know from lived experience.
Is Perimenopause Dizziness Dangerous?
When Dizziness Is Just Hormonal
In the vast majority of cases, perimenopause-related dizziness is uncomfortable but not dangerous. It tends to:
Come and go
Last seconds to minutes (not hours)
Improve with rest, food, or hydration
Not be accompanied by neurological symptoms like slurred speech, facial drooping, or severe headache
It can, however, affect your quality of life, confidence, and willingness to drive, exercise, or participate in daily activities. That impact is real and worth addressing — even if the symptom itself isn't medically "serious."
Red Flags That Deserve Medical Attention
Please see a healthcare provider if your dizziness:
Is sudden, severe, and persistent (lasting hours or days)
Is accompanied by hearing loss, ringing in the ears, or double vision
Comes with chest pain, shortness of breath, or a racing heart
Includes weakness or numbness on one side of the body
Results in fainting or loss of consciousness
Is getting progressively worse over time
These symptoms may point to conditions unrelated to perimenopause — such as BPPV (benign paroxysmal positional vertigo), Ménière's disease, cardiovascular issues, or vestibular migraine — and they deserve proper evaluation.
Can Perimenopause Cause Vertigo?
Dizziness vs. Vertigo — What's the Difference?
These terms are often used interchangeably, but they describe different experiences:
Dizziness = a general feeling of being lightheaded, unsteady, or "off"
Vertigo = a specific sensation that you or your surroundings are spinning or moving
Both can occur during perimenopause. Dizziness is more common. True vertigo is less frequent but does happen — and can be particularly distressing.
Hormonal Vertigo: What We Know So Far
Some researchers have proposed the concept of "hormonal vertigo" — vertigo episodes triggered by hormonal fluctuations rather than structural inner ear problems.
This is most commonly seen in the context of vestibular migraine, a condition where migraine activity affects the balance centers of the brain. Vestibular migraines often worsen during perimenopause, even in women who never had migraines before.
If you experience recurrent vertigo episodes — especially if they come with sensitivity to light, sound, or motion — it's worth discussing vestibular migraine with your doctor.
How Long Does Perimenopause Dizziness Last?
There's no single answer, because every woman's hormonal timeline is different. However, general patterns include:
Individual episodes usually last seconds to a few minutes. Rarely more than an hour.
The symptom as a whole tends to be most intense during mid-perimenopause, when hormonal fluctuations are at their most erratic.
Many women report improvement as they move through the transition and hormone levels stabilize — either naturally into postmenopause or with the support of hormone therapy.
Lifestyle interventions (addressed below) can reduce frequency and intensity significantly, even before hormones fully settle.
The unpredictability can feel overwhelming. But for most women, this is a phase — not a permanent state.
10 Gentle Ways to Manage Perimenopause Dizziness
You don't have to just "wait it out." There are practical, evidence-informed strategies that can help reduce both the frequency and intensity of dizziness episodes.
Nutrition and Blood Sugar Stability
Eat balanced meals every 3–4 hours. Pair protein, healthy fat, and fiber at every meal to prevent blood sugar crashes. Think: eggs with avocado and greens, not cereal and juice.
Reduce refined sugar and simple carbs. These cause rapid blood sugar spikes followed by crashes — a common dizziness trigger during perimenopause.
Don't skip breakfast. Cortisol is highest in the morning. Eating within an hour of waking helps stabilize both blood sugar and stress hormones.
Hydration, Movement, and Vestibular Health
Stay consistently hydrated. Dehydration worsens dizziness, and perimenopausal women often underestimate their fluid needs — especially if night sweats are present. Aim for at least 2 liters daily.
Move regularly, but gently. Walking, yoga, tai chi, and swimming all support vestibular function and circulation without overstressing the system. Avoid sudden position changes during exercise.
Try vestibular exercises. Simple balance-training exercises (like standing on one foot, slow head turns, or the Epley maneuver for positional vertigo) can help recalibrate your inner ear over time.
Stress Regulation and Sleep Hygiene
Practice slow breathing during episodes. When dizziness strikes, sit down, plant your feet, and breathe slowly (4 counts in, 6 counts out). This calms the autonomic nervous system and often resolves the episode faster.
Prioritize sleep quality. Poor sleep amplifies every perimenopause symptom, including dizziness. Keep the bedroom cool, limit screens before bed, and consider magnesium glycinate, which supports both sleep and nervous system function.
Address anxiety directly. If anxiety is a co-occurring factor (and it often is), consider cognitive behavioral therapy (CBT), mindfulness practices, or speaking with a provider about whether targeted support might help.
When to Consider Medical Support
Talk to your doctor about hormonal and non-hormonal options. If dizziness is significantly affecting your quality of life, medical interventions may include:
Hormone therapy (HT) — which may help stabilize estrogen-related dizziness
Vestibular rehabilitation therapy — a specialized form of physical therapy for balance disorders
Migraine-specific treatment — if vestibular migraine is suspected
Medication review — some medications (blood pressure meds, SSRIs, antihistamines) can worsen dizziness
There is no shame in asking for help. Perimenopause symptoms deserve the same medical attention as any other health concern.
Frequently Asked Questions
Is dizziness a common symptom of perimenopause?
Yes. While not as widely discussed as hot flashes, dizziness is reported by many women during perimenopause. Fluctuating estrogen levels can affect the inner ear, blood sugar regulation, and nervous system — all of which contribute to dizziness.
Can low estrogen cause dizziness?
It can. Estrogen receptors exist in the vestibular system (inner ear), and drops in estrogen may disrupt fluid balance and nerve signaling in the structures responsible for equilibrium.
What does perimenopause dizziness feel like?
It varies. Some women feel lightheaded or "floaty." Others experience brief room-spinning (vertigo), unsteadiness while walking, or wooziness connected to hot flashes or missed meals.
How long does perimenopause dizziness last?
Individual episodes typically last seconds to minutes. The symptom overall tends to be most active during mid-perimenopause and often improves as hormone levels stabilize into postmenopause.
Should I see a doctor for perimenopause dizziness?
If dizziness is recurrent, severe, or comes with hearing loss, chest pain, fainting, or neurological symptoms, yes — see a provider. For milder episodes, lifestyle strategies and hormonal support can often help.
Can perimenopause cause vertigo?
It can. True vertigo (a spinning sensation) is less common than general dizziness but does occur — sometimes linked to vestibular migraine, which is known to worsen during hormonal transitions.
You're Not Imagining This — and You're Not Alone
If you've landed on this page because the room has been tilting and nobody can tell you why — please know this: perimenopause dizziness is real, it's common, and it's explainable.
It doesn't mean something is terribly wrong. It means your body is navigating a major hormonal transition, and your balance system is sensitive to the ride.
You deserve information. You deserve validation. And you deserve strategies that actually help.
Start with the basics — steady blood sugar, hydration, rest, movement. If it persists, advocate for yourself with your healthcare provider. Bring this article. Bring your notes. Bring your questions.
You're not "just stressed." You're not "too young for this." You're in perimenopause, and your symptoms matter.
Ready to take the next step?
(https://perimenopausecompass.com/free-14-day-tracker) to find your personal triggers.
Get the Perimenopause Nutrition Protocol to support your nervous system from the inside out.
Visit our (https://perimenopausecompass.com/start-here) page for more foundational guidance.
Get the Perimenopause Nutrition Protocol ($29 + bonus) → https://perimenopausecompass.gumroad.com/l/iecoc
______________________________________
Disclaimer Education only — not medical advice. Consult a qualified healthcare professional for diagnosis and treatment.
Sources / References
Perimenopause Compass
Contact
hello@perimenopausecompass.com
© 2026 All rights reserved.
