How Long Does Perimenopause Last? Timeline and Sleep Guide
How long does perimenopause last? The honest answer: it depends. Explore a realistic year-by-year timeline, what shapes your experience, and how to navigate each phase with clarity.
EDUCATIONAL
Perimenopause Compasss
2/1/202618 min read
You've accepted that perimenopause is happening. You understand the symptoms. You're managing — some days better than others.
But there's one question that surfaces at 2 a.m. between the night sweat and the racing thoughts:
How long is this going to last?
It's a fair question. And you deserve more than "4 to 10 years" as an answer.
If you've Googled "how long does perimenopause last," you've already discovered that most articles give you a medical range, a vague reassurance, and move on. That's not enough. Because living inside this transition — day after day, month after month, year after year — requires more than a statistic. It requires context, honesty, and a map.
This article gives you that map. A realistic, phase-by-phase timeline based on clinical research and real women's experiences — so you can understand not just how long perimenopause lasts, but what each stage actually looks and feels like, what influences your personal timeline, and how to navigate it with less uncertainty.
The Short Answer (And Why It's Not Enough)
The Medical Range — 4 to 10 Years
Let's get the clinical answer on the table first:
Perimenopause lasts an average of 4 to 8 years, with some women experiencing the transition for as few as 2 years and others for 10 years or longer.
The average age of menopause (your final menstrual period) is 51 in the United States and UK. Since perimenopause precedes menopause, it typically begins in the mid-40s — though onset in the late 30s or early 40s is well within normal range.
Here's the data at a glance:
Download the free 14-day tracker
_____________________________________
Disclaimer Education only — not medical advice. Consult a qualified healthcare professional for diagnosis and treatment.
Sources / References
Why That Range Feels Useless When You're Living It
"4 to 10 years" is a six-year gap. That's the difference between a transition that started at 44 ending at 48 — versus lasting until 54. Those are fundamentally different life experiences.
And the range doesn't tell you:
Where you are right now — early, middle, or late in the process
Whether your symptoms will stay the same, get worse, or improve
What actually happens during each phase — how the experience evolves
What factors might make your journey shorter or longer
When you'll know it's ending — or whether it already has
The honest truth is: no one can tell you exactly how long your perimenopause will last. Not your doctor, not a blood test, not an app.
But what we can do is give you a detailed, realistic map of the terrain — so you know what to expect at each stage, even if you don't know your exact exit date.
The Perimenopause Timeline Most Doctors Don't Explain
Most medical resources describe perimenopause as a single block of time. But women who've lived through it — and the research that tracks them — tell a different story.
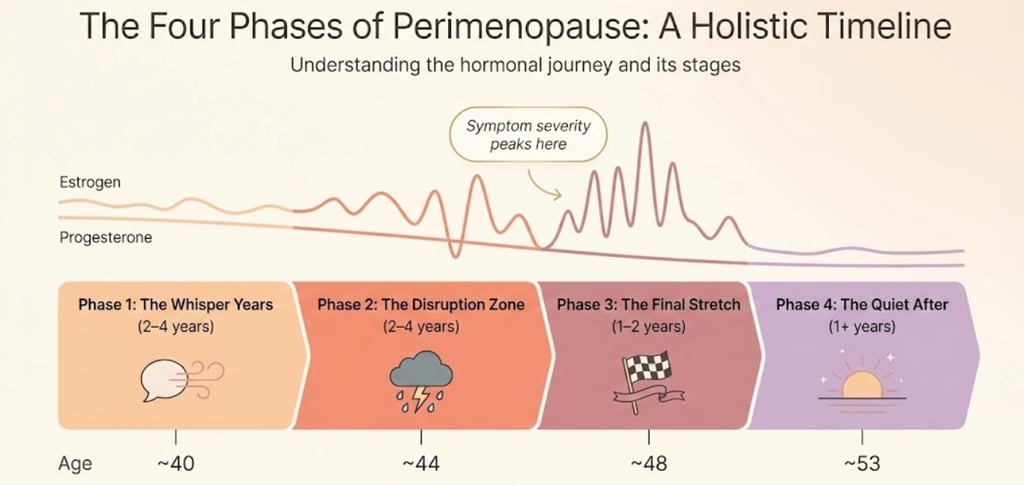
Perimenopause unfolds in recognizable phases, each with its own hormonal signature and symptom profile. Understanding these phases is the closest thing to a timeline that's actually useful.
Phase 1 — The Whisper Years (2–4 Years Before You Notice)
Approximate timing: Often begins in the early-to-mid 40s (sometimes late 30s)
Duration: Typically 2–4 years
What's happening hormonally: Progesterone begins declining as ovulation becomes subtly inconsistent. Estrogen is still mostly in range — sometimes spiking higher than normal. FSH may start to creep up but fluctuates significantly.
What you might notice:
Your cycles are slightly shorter — maybe 25–26 days instead of 28–30
PMS feels a bit more intense
Sleep quality has shifted — not dramatically, but something is different
You're a little more anxious, or a little more tired, or a little more emotionally reactive
You have a vague sense that something has changed — but nothing you can pinpoint
What you probably DON'T notice:
You're not connecting these subtle shifts to hormones
Each symptom in isolation seems explainable — stress, age, busy life
You likely haven't said the word "perimenopause" yet
Why this phase matters: These are the years most women lose to confusion. They're experiencing real hormonal changes, but the symptoms are too quiet to trigger recognition. Many women look back later and realize: "Oh — it actually started three years before I thought it did."
This is the phase where education makes the biggest difference. If you recognize the whispers, you can start tracking, adapting, and preparing — instead of spending years wondering what's wrong.
Phase 2 — The Disruption Zone (The 2–4 Years You Feel It Most)
Approximate timing: Typically mid-to-late 40s
Duration: Usually 2–4 years (this is the "active" phase most women identify as "perimenopause")
What's happening hormonally: Estrogen enters its characteristic roller coaster — spiking unpredictably (sometimes to levels higher than your 20s), then crashing. Progesterone continues declining. Ovulation becomes increasingly irregular. FSH is rising but still variable.
What you experience:
Cycles become visibly irregular — varying by 7+ days month to month, occasionally skipping
Hot flashes and night sweats emerge or intensify
Sleep disruption becomes a regular problem — not occasional, but most nights
Anxiety, mood swings, or irritability feel impossible to manage with your usual coping strategies
Brain fog affects your daily functioning — work, conversations, memory
Fatigue becomes persistent and resistant to rest
Physical symptoms multiply — joint pain, headaches, palpitations, weight redistribution, vaginal dryness
What makes this phase so hard:
This is the phase that brings women to their doctors, to Google, and sometimes to tears. The intensity can be overwhelming — and it often hits during one of the busiest, most demanding decades of life (career, parenting, aging parents, relationships).
The cruel irony of Phase 2: you finally know what's happening, but knowing doesn't make it easy.
The important thing to understand: Phase 2 does not last forever, even when it feels like it might. Research consistently shows that symptom severity typically peaks in the 1–2 years surrounding the final menstrual period — then gradually diminishes. You are not stuck permanently in the worst of it.
Phase 3 — The Final Stretch (1–2 Years Before Menopause)
Approximate timing: Typically late 40s to early 50s
Duration: Approximately 1–2 years
What's happening hormonally: Estrogen fluctuations are widening to their most extreme range. Periods may disappear for 2–3 months, then return unexpectedly. Your body is approaching its final menstrual period — though you won't know it was the last one until 12 months have passed.
What you experience:
Long gaps between periods — 60, 90, sometimes 120+ days
When periods return, they can be unpredictable — very heavy, very light, or different from anything you've experienced before
Vasomotor symptoms may peak — this is often the most intense window for hot flashes and night sweats
Some women experience a shift in symptom quality — anxiety may evolve into a more chronic, low-level hum rather than acute attacks
There may be moments of unexpected relief — good weeks or even good months that make you wonder if it's over
New symptoms may emerge — vaginal and urinary changes often become more noticeable in this phase as estrogen levels trend consistently lower
The emotional landscape:
Phase 3 carries a unique emotional signature. There's often a mix of exhaustion and anticipation — the fatigue of years of symptoms alongside the hope that the end is approaching. Some women describe a sense of mourning — for their reproductive years, their younger body, or simply the self they were before perimenopause changed things.
These feelings are normal. They don't require fixing. They deserve acknowledgment.
Phase 4 — The Quiet After (The First Year of Postmenopause)
Approximate timing: The 12 months following your final menstrual period (though you won't confirm it until month 13)
Duration: 12 months (by definition) — but the hormonal settling continues for 1–2 years
What's happening hormonally: Estrogen and progesterone stabilize at their new, lower baseline. FSH remains elevated. The dramatic fluctuations of perimenopause are over. Your body is recalibrating.
What you experience:
Vasomotor symptoms typically begin to decrease — though some women continue to have hot flashes for years after menopause (research from the SWAN study found that the median total duration of hot flashes is 7.4 years, with some women experiencing them for 10+)
Sleep may begin to improve — though postmenopausal sleep is not always identical to pre-perimenopausal sleep
Brain fog often lifts — many women report a gradual cognitive clearing in the first 1–2 years post-menopause
Mood stabilizes — the emotional volatility of perimenopause tends to calm as hormones stop fluctuating
Vaginal and urinary symptoms may persist or worsen — these are driven by sustained low estrogen and often require ongoing management (local estrogen therapy can be very effective)
Some women describe feeling like themselves again — or like a new version of themselves
The recalibration paradox: Not everything resolves immediately. Some symptoms improve rapidly once fluctuations stop. Others — especially genitourinary symptoms, bone density changes, and cardiovascular risk — are long-term considerations that benefit from ongoing attention.
Menopause isn't an ending. It's a new hormonal baseline. And for many women, once the storm of perimenopause passes, there's a genuine sense of relief, stability, and even renewal.
What Determines How Long YOUR Perimenopause Will Last?
This is the question behind the question. You're not asking how long perimenopause lasts in general — you're asking how long it will last for you.
While no one can give you an exact answer, research has identified several factors that influence both duration and severity.
Genetics — Your Mother's Timeline Matters
Your genes are the single strongest predictor of your menopause timing.
Research published in Human Reproduction shows that the age at which your mother reached menopause is a significant predictor of when you will. If your mother went through menopause at 48, you're more likely to have a similar timeline than a woman whose mother went through it at 55.
What to do with this:
If you know when your mother (or older sisters) went through menopause, you have a rough target window
If you don't know — ask, if possible. It's one of the most useful pieces of health information a woman can have
Remember: it's a predictor, not a guarantee. Other factors can shift your timing by several years
Ethnicity and Racial Differences in Duration
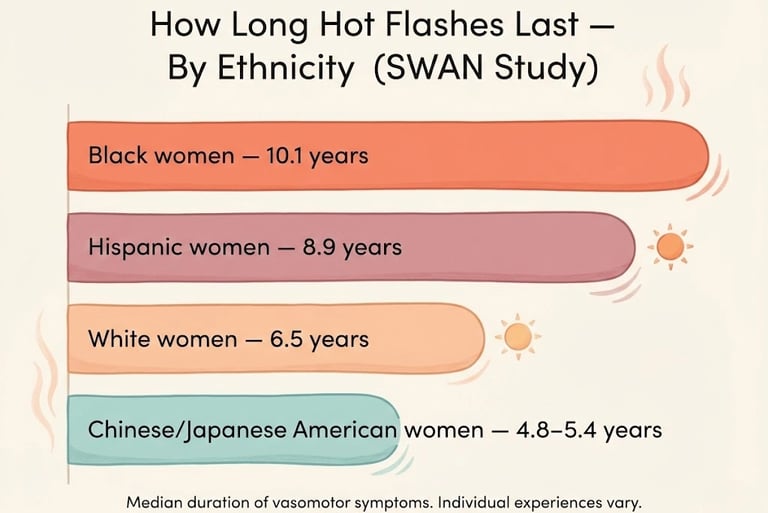
The SWAN study — the largest longitudinal study of the menopausal transition — found significant differences in both timing and symptom experience across racial and ethnic groups:
These differences are real, significant, and under-discussed. If you're a Black or Hispanic woman and your perimenopause feels like it's lasting longer than what articles describe — it's not your imagination. The research confirms that your experience may genuinely be longer and more intense, and your care should reflect that.
Lifestyle Factors That Influence Length and Severity
While you can't change your genetics or ethnicity, certain lifestyle factors are associated with both the timing and severity of perimenopause:
Factors associated with EARLIER menopause (and potentially shorter total timeline):
Current smoking (the most consistent modifiable factor — smokers reach menopause an average of 1–2 years earlier)
Lower body mass index
Higher chronic stress levels
History of certain chemotherapy treatments
Factors associated with LATER menopause (and potentially longer total timeline):
Higher body mass index (fat tissue produces estrone, a form of estrogen)
Multiparity (having had multiple pregnancies)
History of oral contraceptive use (possibly)
Factors associated with REDUCED symptom severity (regardless of duration):
Regular physical exercise — especially strength training and moderate cardio
Healthy dietary patterns (Mediterranean-style, anti-inflammatory)
Not smoking
Lower alcohol consumption
Effective stress management
Adequate sleep support
The takeaway: You can't choose how long your perimenopause lasts. But you can significantly influence how much it disrupts your life during that time.
Surgical and Medical Factors
Certain medical situations alter the perimenopause timeline dramatically:
Bilateral oophorectomy (removal of both ovaries): Causes immediate surgical menopause — no gradual transition. Symptoms can be abrupt and severe due to the sudden loss of hormones.
Hysterectomy with ovary preservation: Removes the visible marker (periods) but leaves ovaries functioning. You'll still go through perimenopause — you just won't have menstrual changes to track it by. This can make it harder to know where you are in the timeline.
Chemotherapy or pelvic radiation: Can damage ovarian function and accelerate the transition.
Endometrial ablation: Reduces or eliminates periods but doesn't affect ovarian hormones. Similar to hysterectomy with preservation — you're perimenopausal but missing the cycle-change markers.
If any of these apply to you, your timeline will look different from the standard phases described above — and you may benefit from more frequent monitoring and earlier discussion of hormone therapy options.
The Stress–Duration Connection
This one is nuanced and still being studied, but it's worth noting.
Chronic psychological stress is associated with:
Earlier onset of perimenopause
Greater symptom severity during the transition
More frequent hot flashes and night sweats (cortisol and the thermoregulatory center in the hypothalamus are closely linked)
Worse sleep outcomes — compounding the effects of hormonal changes
Stress doesn't "cause" perimenopause. But it can amplify it — making the same hormonal fluctuations feel more disruptive and harder to manage.
This isn't said to blame you for your stress levels. It's said because it reframes stress management from a "nice to have" into a legitimate medical strategy for navigating perimenopause.
What Women Actually Experience — Year by Year
Medical timelines are useful. But they don't capture the texture of living through this transition. Here's what the journey actually sounds like when women describe it in their own words:
"Year 1–2: I Didn't Even Know It Had Started"
"At 43, my periods got a little shorter. Maybe 25 days instead of 28. I was more tired than usual, sleeping less deeply, and my PMS was noticeably worse — I was crying at commercials, which was not like me. But I explained it all away. Work was stressful. The kids were young. I was just 'getting older.' It never occurred to me that perimenopause had already begun. Looking back, it was so obvious. But in the moment, there was no reason to connect the dots."
"Year 3–4: Everything Intensified"
"By 45, it was impossible to ignore. I was having night sweats three or four times a week. My anxiety went from background noise to a daily battle. I couldn't concentrate at work — I'd lose words mid-sentence, forget what I walked into a room for, read emails three times without absorbing them. My periods were all over the place — 22 days one month, 35 the next. I finally saw a menopause specialist who said, 'You're right in the thick of it.' Oddly, that was comforting. At least I wasn't losing my mind."
"Year 5–6: I Finally Found What Worked — Then It Shifted Again"
"This was the frustrating part. I'd figured out what helped — HRT, better sleep routine, less alcohol, more protein. And for about six months, I felt like myself again. Then my symptoms shifted. The hot flashes calmed down but the joint pain arrived. The anxiety faded but a heavy fatigue took its place. It was like playing whack-a-mole with hormones. My doctor reminded me: perimenopause isn't linear. Your hormones are still fluctuating, and the pattern changes. That helped me stop expecting it to be a straight line."
"Year 7+: The Slow Fade"
"I'm 51 now, and I haven't had a period in nine months. I'm cautiously optimistic. The night sweats have gone from nightly to once a week. My sleep is better — not perfect, but better. The brain fog has cleared significantly. I still have days where I feel the hormonal echo — a wave of heat, a flash of irritability — but it's not running my life anymore. My doctor says I'm likely in the home stretch. And for the first time in years, I feel like I can see the other side."
What Science Says About Perimenopause Duration
The SWAN Study — The Most Comprehensive Data We Have
The Study of Women's Health Across the Nation (SWAN) is the most important longitudinal study on the menopausal transition. It followed over 3,300 women of diverse racial and ethnic backgrounds for more than 20 years, tracking hormonal changes, symptoms, and health outcomes.
Key findings relevant to perimenopause duration:
The median duration of the menopausal transition (from first menstrual irregularity to final menstrual period) is approximately 4–5 years
The median total duration of vasomotor symptoms (hot flashes and night sweats) is 7.4 years — significantly longer than previously thought
Vasomotor symptoms that begin in early perimenopause tend to last longer than those beginning closer to menopause
Symptom duration varies significantly by race/ethnicity (see the ethnicity section above)
Women who experience their first hot flash before their final menstrual period have a longer total duration of symptoms than women whose symptoms begin after
What this means for you: If you've been told hot flashes "last about 2 years," that's outdated. For many women, vasomotor symptoms persist well beyond menopause — though they typically decrease in frequency and intensity over time.
How the STRAW+10 System Maps the Timeline
The Stages of Reproductive Aging Workshop (STRAW+10) provides the most widely used clinical framework for mapping where a woman is in the menopausal transition:
These numbers are clinically accurate. And clinically inadequate.
How to use this: If your cycles have just started varying (more than 7 days from your usual length), you're likely in Stage -2 (early transition). If you've experienced gaps of 60+ days, you've likely moved into Stage -1 (late transition). This doesn't tell you exactly how long you have left — but it tells you where you are on the map.
What's Established vs. What We're Still Learning
Scientifically established:
Average perimenopause duration is 4–8 years; range extends from 2–12+ years
Symptom severity typically peaks in the 1–2 years surrounding the final menstrual period
Vasomotor symptoms last a median of 7.4 years (SWAN data)
Genetics, ethnicity, BMI, and smoking status influence timing
Clinical diagnosis (symptoms + cycle changes) is more reliable than blood tests
Probable (growing evidence):
Earlier symptom onset correlates with longer total symptom duration
Psychological stress may accelerate onset and increase symptom severity
Gut microbiome health influences symptom experience
Exercise and dietary patterns can meaningfully reduce severity (if not duration)
Still debated or under-researched:
Whether interventions (HRT, lifestyle changes) can alter the duration of perimenopause itself
Optimal prediction models for individual timeline estimation
The role of environmental exposures (endocrine disruptors) in timing
Long-term cognitive and cardiovascular implications of extended perimenopause
This article is for educational purposes and does not replace medical advice. If your symptoms are significantly affecting your quality of life — regardless of where you are in the timeline — consult a healthcare provider.
What If My Perimenopause Feels Endless?
When the Timeline Feels Longer Than It Should
Some women feel like their perimenopause has been going on much longer than any article or statistic suggests. If that's you, a few possibilities are worth considering:
1. It actually started earlier than you realized.
The Whisper Years (Phase 1) can begin in your late 30s or early 40s without clear recognition. If you look back and connect the dots — the sleep changes at 41, the anxiety at 42, the cycle shifts at 43 — your actual start date may be years before you "officially" noticed.
2. Your symptom pattern may be evolving, not repeating.
Perimenopause isn't one symptom experience on repeat. The symptoms change over time. If new symptoms keep emerging, it can feel like it's starting over — when in fact, it's progressing. This is particularly true of the Phase 2 → Phase 3 transition, where vasomotor symptoms may intensify even as mood symptoms shift.
3. Something else may be contributing.
Conditions that can extend or amplify what feels like perimenopause include thyroid dysfunction, chronic stress or adrenal fatigue, autoimmune conditions, and depression or anxiety disorders. These can coexist with perimenopause, making the experience feel more prolonged and severe than hormonal changes alone would cause.
Conditions That Can Extend or Mimic Prolonged Perimenopause
If your perimenopause feels unrelenting — or if treatment isn't helping as expected — ask your provider to screen for coexisting conditions. The most comprehensive care addresses all contributing factors, not just hormones.
When to Seek a Second Opinion
Consider seeking a second opinion — ideally from a menopause specialist or NAMS-certified practitioner — if:
Your symptoms have been unmanaged for more than 6–12 months despite raising them with your doctor
You've been told you're "too young" for perimenopause (despite symptoms consistent with it)
Treatment has been ineffective or inappropriate (e.g., prescribed antidepressants without hormonal assessment)
You feel dismissed, unheard, or gaslit about your experience
You have complex medical history (surgical menopause, cancer history, autoimmune conditions)
You have the right to care that takes your symptoms seriously and considers the full picture — hormonal, medical, and psychological.
Can You Shorten Perimenopause?
The Honest Answer About Duration
No. You cannot meaningfully shorten perimenopause.
The duration of the transition is primarily determined by your biology — your genetics, your ovarian reserve, and the rate at which your body's hormonal production declines. No supplement, diet, or lifestyle intervention has been shown to accelerate the transition itself.
Any product or program that promises to "speed up" perimenopause or "get through it faster" is, at best, misleading.
What You CAN Control — Reducing Symptom Severity
You can't control how long perimenopause lasts. But you can dramatically influence how much it impacts your daily life.
Evidence-based strategies that reduce symptom severity:
The reframe: Instead of asking "How can I make this shorter?" ask "How can I make this more liveable?" That question has real, actionable, evidence-based answers.
🔎 Tools and Resources That Help You Navigate the Timeline
This article may contain affiliate links. We only recommend products we've researched and believe may be genuinely useful for women in perimenopause. Affiliate commissions help support this site at no extra cost to you.
1. Balance App (by Dr. Louise Newson)
Best for: Free symptom tracking with generated health reports for doctor appointments
Why it helps: Tracks symptoms over time, showing patterns and progression through the transition phases — exactly the data you need when asking "where am I in my timeline?"
Strengths: Free, medically informed, available worldwide
Limitations: UK-developed content; some features may not reflect US healthcare pathways
2. "The Menopause Manifesto" by Dr. Jen Gunter
Best for: Women who want the definitive, evidence-based book on the full menopausal transition — including timeline, treatment options, and debunked myths
Why it helps: Written by a renowned OB-GYN, this book covers the science of perimenopause and menopause with clarity and authority. Excellent chapter on what to expect and when
Strengths: Rigorous science, empowering tone, myth-busting, comprehensive
Limitations: Dense for casual readers; one clinical perspective
3. "The New Menopause" by Dr. Mary Claire Haver
Best for: Women who want practical protocols alongside medical knowledge — especially nutrition, HRT considerations, and lifestyle adjustments
Why it helps: Combines the Galveston Diet approach with menopause medicine. Particularly useful for understanding how nutrition and exercise interact with the perimenopause timeline
Strengths: Action-oriented, accessible, addresses weight and body composition changes
Limitations: One approach — always complement with individual medical guidance
4. Oura Ring (Gen 3)
Best for: Objective sleep and biometric tracking across the perimenopause timeline
Why it helps: Tracks body temperature trends, sleep architecture, and heart rate variability — all of which shift during perimenopause. Over months, this data reveals how your transition is progressing and whether interventions are working
Strengths: Objective data, temperature trends correlate with hormonal patterns, excellent sleep analytics
Limitations: $299+ investment, subscription required for full features, correlative not diagnostic
5. Magnesium Glycinate (200–400 mg)
Best for: Sleep support, muscle relaxation, anxiety reduction as complementary support throughout the timeline
Why it may help: Magnesium supports GABA activity and muscle relaxation. Many perimenopausal women are deficient without realizing it. Best taken 30–60 minutes before bed
Evidence level: Modest but positive for sleep quality. Low risk for most people
Look for: Third-party tested (USP, NSF) — quality varies significantly across brands
Limitations: Not a substitute for medical treatment of significant symptoms. Results vary individually. Discuss with your provider if you take medications
YMYL disclosure: No tool, book, or supplement replaces personalized medical care. These resources are recommended as supportive aids alongside — not instead of — guidance from a qualified healthcare provider. Individual experiences vary.
How to Know Where You Are in Your Timeline
Markers That Indicate Early, Mid, and Late Transition
You can't pinpoint your exact position with certainty, but these markers can help you estimate where you are:
You're likely in EARLY transition if:
☐ Your cycles have shortened or become slightly unpredictable
☐ Symptoms are subtle — sleep changes, mood shifts, increased PMS
☐ You haven't skipped a period yet
☐ You're between 38 and 45
You're likely in MID transition if:
☐ Cycles vary significantly — sometimes short, sometimes long, occasionally skipped
☐ Hot flashes and/or night sweats have emerged
☐ Multiple symptoms are affecting daily life (sleep, mood, cognition, energy)
☐ You're between 44 and 50
You're likely in LATE transition if:
☐ You've had gaps of 60+ days between periods
☐ Periods are infrequent and unpredictable when they occur
☐ Vasomotor symptoms may be at their peak (or beginning to shift)
☐ You're between 48 and 55
You may have reached menopause if:
☐ It has been 12 consecutive months since your last period
☐ You're experiencing symptom stabilization — things feel different from the acute phase
☐ You're typically 50+ (but range is 45–58)
⚠️ If you've had a hysterectomy (with ovary preservation), endometrial ablation, or use a hormonal IUD — you've lost the menstrual cycle marker. In this case, tracking symptoms over time and discussing with a provider are your best tools for estimating timeline position.
Tracking Your Way to Clarity
If you want to understand where you are in your timeline, consistent tracking is your most powerful tool.
Track daily for at least 4–8 weeks:
Cycle day (if menstruating)
Sleep quality (1–5)
Energy (1–5)
Hot flashes/night sweats (frequency and intensity)
Mood (dominant emotions)
Physical symptoms (joint pain, headaches, palpitations, etc.)
Notable factors (stress, alcohol, exercise)
After tracking, review your log with these questions:
Are my cycles changing in length or regularity? (Early → mid indicator)
Do I have vasomotor symptoms? How frequent? (Mid → late indicator)
Have I skipped any periods for 60+ days? (Late indicator)
Are symptoms stable, worsening, or shifting? (Helps assess progression)
This data is also invaluable for your doctor — it provides the clinical picture that a blood test cannot.
The Timeline Isn't the Whole Story
Here's something that no timeline article tells you — but that every woman who's lived through perimenopause eventually discovers:
The duration matters less than you think.
Yes, it's natural to want to know when it will end. The uncertainty is exhausting. But the women who navigate perimenopause with the most resilience and the least suffering aren't the ones who got lucky with a shorter timeline. They're the ones who:
Recognized their symptoms early and stopped blaming themselves
Found a healthcare provider who took them seriously
Built a support system — medical, personal, and informational
Made peace with imperfection — accepting that some days will be harder than others
Took action where they could (nutrition, exercise, sleep, stress, HRT) and released control where they couldn't (duration, timing, exact trajectory)
Perimenopause is not a countdown to endure. It's a transition to navigate. And how you navigate it matters far more than how long it takes.
You're not waiting for it to end. You're learning how to live well through it — and beyond it.
FAQ — How Long Does Perimenopause Last?
Q: How long does perimenopause last on average?
A: Perimenopause lasts an average of 4 to 8 years, though the range extends from 2 to 12+ years. Duration is influenced by genetics, ethnicity, smoking status, and body composition. Symptom severity typically peaks in the 1–2 years surrounding the final menstrual period.
Q: Can perimenopause last 10 years or more?
A: Yes. While less common, some women experience perimenopause for 10 to 12+ years. The SWAN study found that vasomotor symptoms alone can last a median of 7.4 years. If symptoms began early (before 45), total duration tends to be longer.
Q: How do I know when perimenopause is ending?
A: Perimenopause ends when you've gone 12 consecutive months without a period — that's the official definition of menopause. Before that, lengthening gaps between periods (60–90+ days) suggest you're in the final phase of the transition.
Q: Does perimenopause get worse before it gets better?
A: Often, yes. Research shows that symptom severity typically peaks in the 1–2 years before the final menstrual period. Many women experience their most intense symptoms in late perimenopause before a gradual improvement after menopause.
Q: Can anything speed up perimenopause?
A: No lifestyle intervention or supplement can meaningfully shorten perimenopause. The timeline is primarily determined by genetics and biology. However, you can significantly reduce symptom severity through hormone therapy, exercise, nutrition, and stress management.
Q: Do hot flashes stop after menopause?
A: Not necessarily. The SWAN study found that the median total duration of hot flashes is 7.4 years, and they often continue into postmenopause. However, they typically decrease in frequency and intensity over time. Some women experience them for 10+ years.
Get the Perimenopause Nutrition Protocol ($29 + bonus) → https://perimenopausecompass.gumroad.com/l/iecoc
Perimenopause Compass
Contact
hello@perimenopausecompass.com
© 2026 All rights reserved.
